A VA OIG report shows the Obama-led VA administration of the Veterans Choice Program found massive overpayments, tardy payments, and erroneous payments.
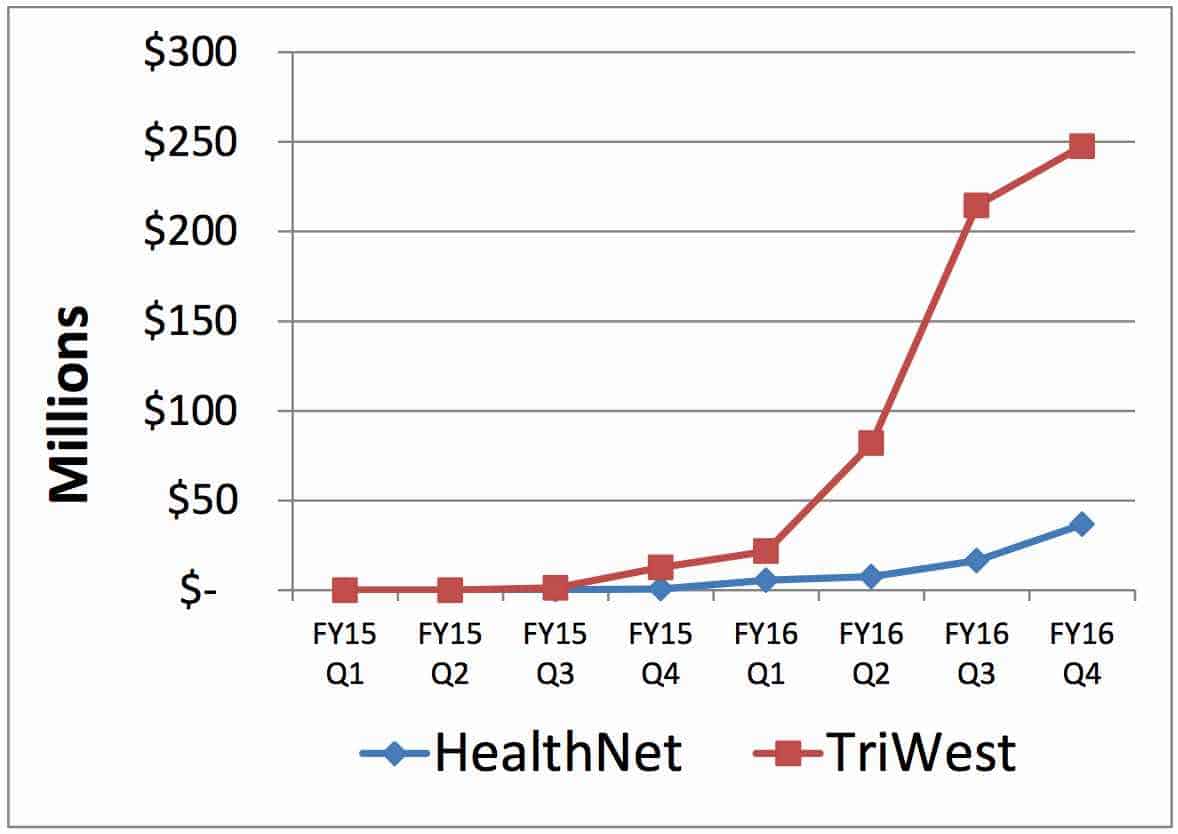
Quietly before Christmas, VA OIG released its report into the administration of the VA Choice Program and its administrators Health Net Federal Services and TriWest Healthcare Alliance Corporation. The report addressed an audit for the period between November 1, 2014, to November 30, 2016. IG found VA overpaid program administrators by $39 million, made 224,000 payments in error, and made another 1 million payments late.
A quick search suggests no major news media outlet covered it directly other than RT.
For some background, President Obama and Congress pushed through VA Veterans Choice Program after VA was caught engaging in outright fraud to increase employee bonuses that caused countless veteran deaths nationwide. The program to this point has largely been a failure due in large part to VA’s failure to properly administer the program.
RELATED: McCain Connection With TriWest
Many veterans believe the failures are intentional to justify maintaining status quo within VA. Meanwhile, certain insiders know VA is allowed to continue failing to further justify eroding the agency’s mission in favor of privatizing the agency, entirely.
The VA Fee Basis Claims System is supposed to administer the Veterans Choice Program through administrators. It has utterly failed to properly administer the program but instead used the failures in other areas to skim money away from Choice to other programs.
RELATED: Veterans Choice Overbilled By Tens Of Millions
VA OIG Audit Of Veterans Choice Program Payments
Here is the executive summary:
Congress required that the OIG report on the accuracy and timeliness of VA payments for medical care provided under Choice. This report addresses payments processed through VA’s Fee Basis Claims System from November 2014 through September 2016. The Veterans Health Administration’s (VHA’s) Office of Community Care (OCC) contracted with Third Party Administrators (TPAs) to process claims and pay Choice medical providers. During the 23-month audit period, OIG sampled from a population of 2 million Choice claims. Of those claims, an estimated 224,000 were paid in error, and 1 million were processed in excess of the 30-day Prompt Payment Standard. The OIG determined weak internal controls over the payment process contributed to these errors. Also, the OCC did not establish clear written policies for Choice claim payments, ensure quality information was available to payment staff, use an information system that could adequately address overpayment of medical claims, establish monitoring activities to determine if payment controls worked, or accurately estimate staffing needs for claims processing. The OIG estimated OCC made $39 million in overpayments to TPAs. The OIG recommended that VHA management ensure systems used for processing medical claims from TPAs have the ability to adjudicate reimbursement rates accurately and issue written payment policies to claims-processing staff. The OIG also recommended that OCC establish expectations and obligations for TPAs that submit invoices for payment, develop sufficient claims-processing capacity to meet expected TPA claim volume, and ensure future TPA contracts contain timeliness standards for processing payments. The Executive in Charge, VHA, concurred and agreed that a full review of Choice payments and recovery of all identified overpayments is essential.
Source: https://www.va.gov/oig/publications/report-summary.asp?id=4006

55 thoughts on “Obama-led VA Overpaid Veterans Choice Contractors By $39 Million, Made 224k Payments In Error, Issued Over 1 Million Payments Late”
Uh oh. Obama isnt going to like this much either. As of 10am this morning AG Sessions has stated that he is overturning Obamas action on medial and rec pot and will start cracking down on them. So far he has closed over 72 shops in New England and has warned Cali to overturn their law or he will come down on them with the full weight of the DOJ and Article 6 Section 2 of the US Constitution (Supremacy Clause which states no lower form of government or court can overturn any portion of the US Constitution-US Supreme Court Decision or legally and Constitutionally passed law by the US Congress) Sounds to me like they are getting serious
“The report addressed an audit for the period between November 1, 2014, to November 30, 2016. IG found VA overpaid program administrators by $39 million…..” $39 million? My conversations with VA “experts” after I spoke to them on the Presidents hotline # reveled it’s more like closer to $500 million (so they think). Yea, a cool half billion $$$.
Healthnet fleeced the living shit out of the VA, and the VA hates them for it, but they are too fucking stupid to call them on that much $$$.
Our friend, “100-0” Shulkin, was too busy sticking his fingers in an electric plug-in socket during this time, which is why he looks the way he does (in every picture). He’s been doing that all his life since he was a little boy, by the way. His brain is really fuckin’ warped and fried by all this voltage and amperage over his life…but he has a medical degree and is a licensed doctor, so he gets away with being a freak. He’s protected. He sticks his fingers elsewhere, too. He really likes being a politician-type these days. He really does. I’m sure he will square out the bilked money going forward with HellNet.
No word about why the Choice referrals went from 3 days to 3 weeks?
Do any of you know where the worst place on earth to be standing is?
I’ll tell you.
It’s standing in between a hungry hungry hippo and it’s bonus check.
…Or a hungry hungry hippo and a Little Debbie delivery truck or Hostess Vending Machine Svc. Vendor refill day at the VA. That would suicide by cellulite. 😀
don’t they have feeder tubes at their station? I thought they just turned their head sideways opened their mouth and pressed a button. Pneumatic Delivery System.
Could you imagine getting in Lasquishas way? Of course I think I’d try it just to see if she managed to operate the damned thing with the 8 inch lacquered claws. Probably just tip it over and start banging on it.
Nope, feeding tube above her workstation like a lab rat, with added benefit of the power & tech behind bank drive-thru teller air-tube delivery systems….**THOOOMP** 😀
maybe we should get somebody to hack her feeding tube and drop a few anvils in her face. ala ACME.
Wow. I cannot understand why no action is taking place to hold people accountable. Ben, I hope they do close the doors on the hospitals.
KimC,
I hope the whole VA, along with the AFGE, is shut down!
I don’t know if I’m eligible for Choice. They sent me a Choice card and then told me I couldn’t use it. That was over three years ago. If I’m eligible for it, being what I’ve read so far about it I’m not sure I want to. If the VA doesn’t pay a provider and then they (the provider) start dunning me for non payment, I don’t think I want any part of it to be quite frank about it. I don’t want the VA ruining my credit rating over its incompetence!
One other thing that came to mind from when my husband was in the emergency room the other day. The “Billing” girl came back into the room where my husband was at and said this to us, “The VA is not paying the bill, so I need your Medicare card” Now, before I go any further, this was all authorized by the VA doctor, he was the one who called the emergency room, and also called VA letting them both know he was sending my husband to the emergency room. My husband is on the Choice Program and he was sent to our local hospital in town by his VA doctor. Now, VA says they are NOT paying the bill and to “Bill” Medicare? Does anyone see what’s going on here? I think I have a clue. VA is billing Medicare first! then, I feel is making up a phony claim and pocketing the money, saying they paid the bill (not telling us that) and making two claims instead of one. This all should have been covered by the VA because it was all authorized by a VA doctor who called the VA and got authorization from them before sending my husband into emergency. Could it possibly be that the VA is billing third party insurance? then filing a claim themselves and pocketing the money of what Medicare pays? I just found this to be very weird when that gal came back to ask for the Medicare card. Maybe they are paying the bill and billing Medicare too. Think about it.
Over the last couple of years, I have had to battle between the VA, Choice and Tri West. I think I know the problem and what’s going on. From several phone calls I had made to these different departments, not any one of them know what the hell they are doing. When I was in communication with Tri West and one of their Customer Relations guy, he told me that between Tri West and VA Choice that they hate each other, do like dealing with each other. Basically, the left hand doesn’t know what the right hand is doing. Now just recently I got in the mail a letter from Healthcare Alliance/ Tri West saying that I have deductibles that need to be met. My husband does not pay deductibles, never has. So I called the number to find out what was going on. Healthcare Alliance told me that this was a mistake made by VA Choice and not them. So basically what that boils down to is, the VA Choice is passing the buck and trying to lay everything on Healthcare Alliance. This guy from Tri West flat out told me that they hate dealing with VA Choice and wished they never got involved in the first place. Bills that the VA is suppose to pay, the VA has been trying to pass it on to Healthcare Alliance. This is what I know from a inside source. This is why I had so many problems with Tri West and getting them to pay the bills. What was happening is, either one of these two places are keeping tabs on each other. VA Choice was not forwarding the paperwork to Tri West, such as the Authorizations for payment process. When I spoke with this guy, he had in his system only “One” authorization, and he told me that he is only paying for the bills for that one authorization. I had all 5 authorizations and faxed every single one of them to him. The bills got paid and never heard another word from him. VA Choice was not on top of things and sending the paperwork to Tri West. It’s crazy!! but I have been dealing with this crap now for 3 years!!
What a mess and huge contributor to PTSD anxiety. But, the VA does not get that they are one of the major ‘triggers’ to Veteran PTSD, while everyone or most at the VA have their craniums up their anuses.
well we all know what the cure for cranial/rectal inversions is yeah?
Actually there are 2!!!
5.56
7.62
I just love getting fuckded by the VA. It makes meez feel like at least someone cares. And when meez get that fuckded by dose fat wide assed RN’s, it lets me know that at least someone wants to fuckded meez, just for meez, and meez alone. But I keep on asking them wide assed, can’t fit through those doors RN’s, to please lets do a test so that I can know if I have feelings on both fronts.
My request; to fuckded me, using @Namnibors special lube w/ grit in it, and apply the unsterile penetrator in the front (small port hole) first, and then to push it deeper so that it dilates in da back, the wider, more flexing port hole, and then with both hands, pull that long unsterile penetrator out from da back endz port hole. And in this manner, I will know that I really have benz fuckded, and this will clarify and demonstrate to Meez that I have feelinz on both fronts. I just lub dose fuckners at the VA. Don’t you agree? Come on now, let us all get fuckdeed.
Oh, and Fuckdeed Meez VA, Fuckdeed Meez AFGE, Fuckdeed Meez DoD, Fuckdeed Meez VSO, come one, come all, and Fuckdeed Meez, please. Don’t forget Nam’s gritty jelly lube.
And you sick fuckdeeds, better give me plenty thumbs up too.
Whilst I can appreciate your anger and frustration, your willingly and voluminously shared details surrounding your virtual penetration issues perhaps belie another deeper issue. Real deep. Might I suggest that it is time for you to embrace the reality of your being a homosexual. Don’t fight it. It’s OK to come out now.
Shhhh sshhh ssshhh ssshhhh…….. Sshh.
And I will not give you my thumb nor any protuberance – up, down, or sideways.
LMFAO. There goes the gossiping now. Should I send the gritty luber stuff back to your reg address, or have you told your love ones yet. lol
Out of 2 million sampled, 224k were paid in error. Does that mean 224k were paid and should not have been? Or is it more likely that means 224k were underpaid or overpaid? Or does it mean there was some other error involved in the payment?
Out of 2 million sampled, a full 50 percent were not paid promptly.
Imagine if you owed the VA. Would they allow you to take your sweet time in getting around to paying it? Or even waiting beyond 30 days to address it?
At least the excuses are familiar. Weak internal controls. Lack of clear policy because common sense doesn’t exist at VA. Need to upgrade our PCs so lets toss in a comment on IT. Ya never know, but maybe we can skim even more if we say our PCs suck.
Claims processing? Am I missing something?
Exactly what is the function of Health Net/TriWest, and what is the function of the VA when it comes to Choice? Veterans have been led to believe the VA authorizes a Choice appointment, then ignores the veteran. Health Net/TriWest finds a provider, schedules the appointment, then processes the providers claim for payment.
If VA is actually processing claims for payment, what is the function of Health Net/TriWest, and why does the VA constantly lie about providers sending the bills to the wrong address at Choice?
If both the VA and Choice are processing claims, its no surprise Shulkin has to demand a couple billion every few months to pay for duplicate claims processing. Which means they process and pay for 1 claim 3 or 4 times before its paid because they both process the claims wrong. Because the policy is unclear and their PCs suck.
@91Veteran- Also begs the question of *just what & why* are ‘Choice Champions’ even needed? Are they there to ensure the triple billing goes unnoticed and smooth as molasses this Winter with the added benefit of another dues-paying AFGE to the herd to show-up and fog a mirror and weight a chair?
If Trump does not fire someone within this year ar VA, he is part of the problem.
Obama never took responsibility for anything at all, that is why you are seeing the effects of his administration and the bubble it created by mass government fraud.
Trump is only worried about $$$ , golf and pussy.
“The tree of Liberty must be refreshed from time to time with the blood of patriots and tyrants. It is it’s natural manure”. Thomas Jefferson
The Liberty tree has had a steady diet of Patriot blood for decades.
FUCK VA, FUCK AFGE
I think AFGE Pres. ‘little’ Cox used ‘The Tree of Liberty’ as a pissing post along with all his dues-paying minions.
Him and his confederates will all be pissing when guys like us put the noose around their necks and pull the knots tight up under the ear.
I’ve read you can braid your own hemp rope and incorporate long dried branches of rose bushes into the twist for a noose that just gives that *extra* zing. 😀
That, Sir, is an excellent little pro tip. See? You learn something new everyday. I’m assuming the thorns are left on? Although why not just hang em with barbed wire use a stool so they suffer as they choke and bleed.
Was trying to be “green” and recycle, but I know for a fact most farmers have excess balls of barbed-wire with and without rust just laying about unused and THAT would classify also as recycling, thus green. I learned something as well. (yes, thorns left on)
Also, sounds like you and I should be the VA OIG’s interrogators. 😀
Can we leave out the “good cop” part and just both be bad cops?
Key words in Bens article, Quietly and Fraud. Imagine that, those two words being associated with VA. Trough feeding fucking scum.
FUCK VA, FUCK AFGE
If they were not quiet about this report, then the public might find out the Choice program is not working like it has been described publicly. If that happens, there MIGHT be some in the public demanding to know why congress keeps shoveling billions at this program, and why nobody has been held accountable.
Or they might just continue to wonder which Kartrashian is spawning.
Let’s see here. “Songbird McCain’s” name is attached in some way with the Choice Program. That, in itself, IS suspicious. Seeing as though his name is being tied to MANY other possible illegal activities as well!
Then, the contractors, OR administrators, get a good chunk of the monies, $39 million, illegally. Which were supposed to be used for veterans healthcare.
Then, for some unexplained “excuse”, monies were NOT paid out to outside healthcare providers. Leaving said veterans to “pick up the tab” for the Choice Program.
IF the veteran didn’t pay, well, that’s ok, choice allowed the late payment to go to a private company, “collection agencies, to insure payment, [Sarcasm intended here]!
Let’s not forget, our duly elected representatives STILL have not held anyone accountable at VA for their actions – YET! Instead, they allowed “Shithead Shulkin” to make fools out of them – AGAIN, by holding veterans healthcare hostage – AGAIN, to demand another $2.1 BILLION DOLLARS from the taxpayers of America – AGAIN.
How many BILLIONS of taxpayers monies has flowed through the Choice Program since its inception? Does anyone actually know WHERE that money has gone? Does anyone know HOW many have opened NEW offshore accounts since its inception? All of my questions are rhetorical! IF there’s one thing veterans suspect it is; – “The Choice Program was set up to fail!
AND,
The Choice Program is, in ALL actuality, a “Slush Fund” set up to financially benefit EVERYONE except veterans SEEKING outside healthcare!
Audit the buck out of the VA. 😀
If, by audit, you mean shoot every VA fuck you can get in your crosshairs until you fire yourself dry, then yeah I’m game.
Now, now…I did not imply ‘buckshot’. 😀 Just a very comprehensive audit.
Well, a good “tight pattern” of rock salt would get the message across!
All I can think about in this deep frigid cold winter weather is that the VA’s overpaid Choice Contractors by $39 MILLION…that would be MORE THAN ENOUGH to END Veteran Homelessness and place a serious dent in helping with Veteran Suicide Prevention.
I also think of all those VA Travel Pay Fraud Warning Posters and how the VA can spot an erroneous DIME….but issues over 1 MILLION PAYMENTS for Choice Medical LATE, placing Veterans in collections…and JUST HOW MANY veteran suicides were prompted by the VA’s nonpayment or refusal to assist?
I’m thinking at this point the Choice Program is actually a VA Suicide Assist PsyOps Program while these fucks maximize their nonperformance bonuses. “Choice” is simply the VA’s “Final Solution” name for it.
I want to point-out a funny linguistic thing: Notice the VA Spokeshack mentions the VA was “late with over 1 million Choice Payments”.
That does NOT mean $1 Million in bills…it means over 1 MILLION individual procedures the VA could give a shit about because it already paid for a new boat, roof, vacation to England, new pool…you get the gist. It’s already in AFGE’s sticky fingers.
The VA is trying to PAD their release by PADDING the language. THAT 1 MILLION individual bills LATE is CODE for…NEVER EVER PAID AND NEVER INTENDED TO…unless caught…which means it’s likely hundreds of millions of $$$$.
The VA requires a taxpayer appointed fiduciary to manage their $$$ and I nominate Benjamin. or hell, my cat could do a better job than these fucks. (my cat DOES require regular use of MMJ vaporizer, which enhances his counting skills)
Many years ago when I was young and just starting out, I worked for a company in their mail room. This company was like the Health Net for a state in that the company accepted claims from providers, verified them, authorized payments, then mailed the checks to providers. I believe it was for state medicaid or other state health programs. All was done on a very tight 30 day schedule. It was the only time in my life I handled checks that were for over $1 million each. In addition to that, we would mail various kinds of claims forms to the providers when they requested them.
Those million dollar checks were not for a single patient. Those million dollar checks were bulk payment for all of the claims submitted by 1 provider for 1 month. Other checks were for as little as under .20 cents because of a claims error, etc., with many under $1000 or just a little over. There were also many in the $5 to $10,000 range.
You are spot on in questioning whether those 1 million claims represent 1 million vets. I bet you are right in that it involves many millions of dollars each.
I know one provider here in CO wrote a letter to vets they had provided care for asking vets to contact our worthless politicians. That provider alone was owed over $2 million.
Since they violate the prompt payment act, can those providers then claim interest on the money owed? I suspect they can.
Your comment prompts another question nam. How many of these overpayments are actually VA paying the initial claim months after the provider submitted it, then finding out later the veteran had already paid it because the provider sent it to collections?
I have no doubt the VA would completely ignore the veteran in that situation and merely claim the provider was overpaid.
The real question is what if no one blew the whistle? It started a call for fleecing.You may have an entire ‘cast” of people being played and paid to enact fraud. Think about it! VA is stealing money after Dr.Footes exposure of fraud and now that exposure generates more fraud dollars they would have never had, not he come forward.
There is the fish in my TunaBeast analogies to VA employees.
Fuck the VA!!! ………..twice and shit!
Shulkin will fuck the taxpayers twice, maybe thrice, by holding Veteran Healthcare HOSTAGE for ANOTHER $2.1 Billion in order to pay the bill$ the previous $2.1 Billion was supposed to pay for but wifey poo wanted Wimbledon…BVA Murphy wanted an Agent Orange Julius Waterslide installed in his pool shaped like an orange barrel…Sen. McCain needed brain surgery at MAYO CLINIC…Veterans? Who?
Vindictive Affairs: The VA Cares!
Word of the Day: Veteran Affails (Elmer Fudd accent)?
So…They KNOW millions were overpaid…Are they gonna go after the contractors to get that money BACK ? ? ? ? ?
Good question Donald. Wonder what the statute of limitations are about that. Or if they can bring the crooks back from places like Belize or Jamaica for trial. lol
My question is, if 50% are paid late anyway, why are their overpayments at all? I could hear the VA excuses claiming they are taking their time processing the claim to get it right, but if that is the case, why are there not 0 overpayments?
Are these overpayments a result of Choice paying 1 claim and the VA paying a duplicate claim? Its more likely these overpayments are a result of a provider submitting a claim waiting 7 months, then submitting another claim after the VA said it was sent to the wrong address? How many of these overpayments are overpayments because a provider had to send multiple claims for payment?
I reread your post above with added benefit of ‘Benny Hill Music’ playing through my frontal lobes and it somehow made sense, even without the baring of chests. 😀
Benny Hill. bestest theme song EVER!!!!!
First thought is that catching fraud to kick-back schemes over any issue is harder than hell to prove. Especially in a state as corrupt as Indiana. Too much goes un-reported and ignored, while other issues remain flushed or secret unless a person is affected by something and experiences how the censoring to covering up works, and works well to keep the people ignorant of some reality.
Privatizing? To me that would be more corporate controls using the same medical institutions/establishments, same attitudes coming out of the medical schools, more medical visas to be used/demanded, more quotas to fill and appease, insurance panels or medical boards, the same collective punishments over pain meds or other meds that can aid some other issue the government sees fit to keep us from…to save us from ourselves, they claim. We’d still have big Pharma and those congressional stockholders to contend with over profits or to depopulate some from the Earth, or out of their hair. Etc. I would like to see some examples of where privatizing something has actually worked. It sure did great to create the worlds largest prison system here and keeping them full of non-violent offenders, kids, political prisoners to the mentally ill. Oh, and for cheap slave labor. And with the wanted/demanded hate speech laws coming and PC-ness we could be imprisoned or fined for complaining about some foreign MD, checking their credentials, or the likes. So where would the win-win situation be if the USA stays on the course it has for generations? None of the status quo with any issue, or those benefiting from corruption, or profiteering wants to see change. Besides that there are too many networks of those bullies, sadist, and sociopaths, that love playing the retaliation and torture games.
Trump could always use the Obama pen for executive orders. If he can use it for foreigners human rights, Israeli bowing, and other’s national concerns, he could use it for veterans. But he won’t.
If the VA, gubbermint, Congress, medical associations, etc., were concerned or care at all about our health care they would listen to some panels of doctors like Elaina George MD.
“https://drelainageorge.com/” Then take some serious action and stay on it till a drastic change is made. Who else would know how sick our system is other than MDs that left the traditional “cartels,” governmental pressures, to practice by their own styles instead following the herd of greedy uncaring, freaks out there today who stray away from patients problems or concerns due to orders from the rulers/tyrants.
Posted about her before and she pulls no punches about the health care “cartels,” Obummer Care, VA, contractors, the AMA, Congress, the courts, to the insurance companies that have ruined health care on all levels. Including bedside manners to physician-patient trust or confidence that is gone. Or of making the patient and our needs first instead of playing politics, high profits, special interest cards, and police force out to get us all for whatever reasons.
The system has been gamed to suit a variety of purposes having nothing to do with the intent of the program and only God and the AFGE elite really know where all that money evaporizes to. Clever VA managers can spot loopholes in laws from 200 feet away and down the hall and the moment you lay yet another way like Choice that they can bastardize so as to muddle the system then you have given them one more way to fleece America. How many more ways are we gonna toss them?
Think about this carefully – Choice program was born because of rampant dishonesty and corruption had blossomed yet again at VA. Then what did we do after conjuring up solution #1724 to fill the promises of America? We put control of the program into the corrupt hands that necessesitated the creation of it in the first place!!! There is NO program at VA free of corruption. Not one!
If VA was ordered to initiate a plan to give a #2 pencil to each vet then within two months the system would be backlogged by millions, overbudget by billions, and congress would demand to know why VA was passing out broken crayons instead, and VA numbers confirming four pencils had been passed out could not be verified but would be enough to satisfy senior management bonus requirements.
America, there is NOTHING good, productive, righteous, healthy, or honest about VA. We have been infiltrated. This is organized crime presented as a public agency and nothing more.
va dc hq va deathcare one big big big federal rico crime racket howw @ why va budget 2018 is is 186 billion $$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$ va sewage rats a dogs in heat for the $$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$$ legal fact va deathcare is rico crime racket !!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!
congress sewear rats will do nothing for vets on death paneles t
Congressmen are nothing but meatball belly fuckboys!
Let me add something from VA themselves and just ask yourself, what kind of organization defends themselves by pointing out how badly they fuck up??? My God in heaven America the following excerpt is from the opening paragraph of VA Roseburg defending themselves against DAMNING charges of misconduct; Trust me I did NOT make this shit up! Look online yourself! This is how they defend themselves as a hospital!!!
From VA Public Relations, Roseburg Oregon
– “The New York Times story is false.
The Roseburg VAHCS is a one-star facility according to SAIL data. On its face, this shows there is no manipulation of data because, if the facility were manipulating data to boost its rating, wouldn’t it be getting a higher score?”
Should I laugh or cry? This is what I mean in that at every level including the level of clear thinking the system is completely corrupted. By this I mean that they point out and cling to their own complete incompetance as a healthcare facility to prove they have done nothing wrong?
As I read it, they are saying they are so shitty at doing their job, they only got one star AFTER manipulating the data.
And they appear to be very proud of that.
Comments are closed.