Do not believe the hype on this one – VA reported $1.1 billion in improper payments to veterans – by “improper” VA OIG does not mean wrong. That means, while true, the game here is hype plus semantics.
This shocking claim from VA OIG’s new report does not mean these payments went to undeserving veterans. It merely means VA did not dot every “i” and cross every “t” for normal payments or overpayments or underpayments.
Let me explain. When I read the headline and first sentence in a newsletter VA sent me, I thought, “Wow, $1 billion in payments were made to veterans who did not deserve the money.” And how could I not think this when the first sentence started off, “VA reported $1.1 billion in improper payments…” However, that is not what the report really says.
What I learned was that VA lumped together all payments, including overpayments and underpayments, into the same totals. VA waited until the appendix to explain that little detail, but I guarantee that Veterans Benefits Haters will hail the VA OIG report as a red flag indicating VA benefits should be cut.
Here is what you need to know.
VA followed an Office of Management and Budget (OMB) circular’s definition in conducting this evaluation. There, OMB mandated defining potentially correct payments to deserving veterans as “improper” based on a variety of things. For example, if VA did not follow the regulations to the letter, even deserved payments must be labeled improper by VA’s simple application of the rules. However, OMB goes a step further, and VA seems to gloss over a detail or two while explaining its findings until the end of the report.
Here is the full OMB Circular A-123 Appendix C definition per VA:
Incorrect amounts are overpayments and underpayments that are made to eligible recipients (including inappropriate denials of payment or service, any payment that does not account for credit for applicable discounts, payments that are for the incorrect amount, and duplicate payments). An improper payment also includes any payment that was made to an ineligible recipient or for an ineligible good or service, or payments for goods services not received (except for such payments authorized by law). In addition, when an agency’s review is unable to discern whether a payment is proper because of insufficient or lack of documentation, this payment must also be considered an improper payment.
What concerns me about this report is that the Department of Veterans Affairs is disseminating VA OIG reports that could mislead casual readers with irresponsible headlines. You know, these are the readers who only read the headline and first paragraph, ie the majority of Americans.
I guarantee you will see a few talking heads on TV talk about how they believe the US should cut veterans benefits.
Yet, I still waiting to see is a report from VA OIG that documents the lack of value taxpayers get in exchange for the billions VA pays to major government contractors every year. Now that would be an amazing read.
In addition to my main semantic gripe about the title and lead paragraph, within the report, some of the conclusions may be a little looser than one would expect.
For example, when describing Compensation overpayments, VA OIG merely extrapolated an overall guess of what the total improper payments are based on a sample. The report claimed that 10 percent of the sample received improper payments.
The term “improper” is defined for VA OIG by the Office of Management and Budget (OMB) as meaning, “when an agency’s review is unable to discern whether a payment was proper as a result of insufficient or a lack of documentation, this payment must be considered an improper payment.” Specifically, the report may have classified correct payments to deserving veterans as “improper” based on semantics.
Further, VA’s focus on Compensation highlighted only a few instances of payments made where VA did not cross a “t”. This means the inspection is more concerned with semantics than with giving Americans a firm understanding of VA’s regulatory problems.
Here is part of what led to that terribly deceptive headline. While reading this, ask yourself if you think the guts of the report justifies the title:
VBA underreported improper payments for its Compensation program. From VBA’s sample of 400 Compensation payments, the OIG reviewed 21 payments related to temporary 100 percent disability evaluations or traumatic brain injury claims. Of the 21 payments reviewed, we identified two related to temporary 100 percent disability evaluations that lacked routine medical examinations required to support veterans’ benefits.
Specifically, VBA policy requires a temporary 100 percent disability evaluation for a service-connected disability following a veteran’s surgery or when specific treatment is needed. At the end of a mandated period of convalescence or treatment, VA Regional Office staff must request a follow-up medical examination to help determine whether to continue the veteran’s 100 percent disability evaluation. VBA did not count the two payments discussed above as improper payments. However, according to OMB Circular A-123, Appendix C, when an agency’s review is unable to discern whether a payment was proper as a result of insufficient or a lack of documentation, this payment must be considered an improper payment.
VBA’s test procedures for the Compensation program did not include a step to check for the medical examinations required to support temporary 100 percent disability evaluations. We recalculated VBA’s improper payment estimate for the Compensation program to include the two additional improper payments. Consequently, the estimate increased from approximately $321 million to $565 million. The improper payment rate also increased from 0.67 percent to 1.17 percent. By the time of our review, a subsequent examination had been completed but a decision was still pending for one claim. An examination had not been completed for the other claim.
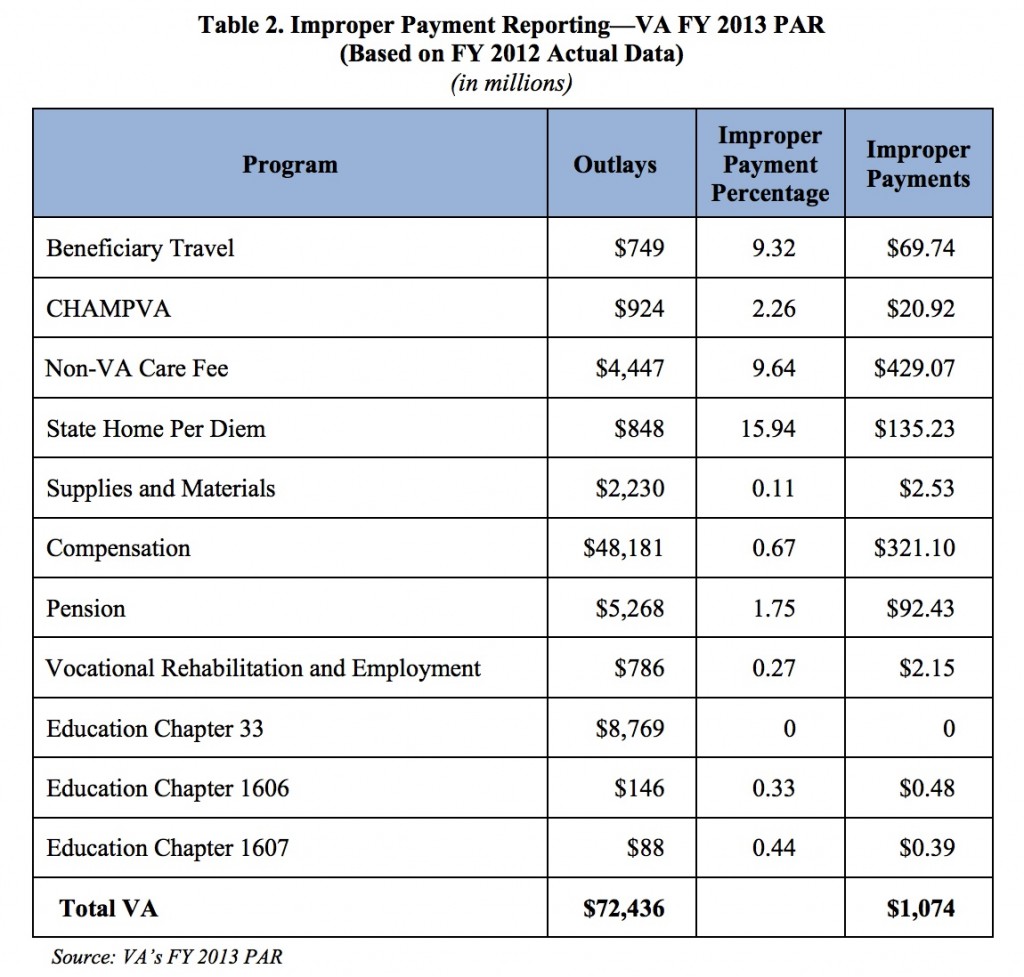
Do you think VA can properly claim $565 million in improper payments based on a mere sample of 400 veterans? Check out this chart on the overall payouts VA OIG evaluated:


17 thoughts on “Truth or Fiction: VA OIG investigated $1.1 Billion in Improper Payments”
The VA is corrupt, 10 year wait for my benefit approval, once approved, they stripped me of all rights, police brutality against me, and the government stole my 6 year old baby. Brutally beaten by police, as a disabled female, and my benefits pension went to x. Don’t waste your time, corrupt, against female Vets, government intrusion, lies, hurt badly …,and I served my country with honor. Stopped of my entire life and will never be the same again after trusting the VA
I am one of those who was paid improperly. Now I am paying back $300 a month for the next ten years. I now realize that I have to be sure to understand what they are doing. That is the hard part cause they don’t know. Now I live extra lean. Before when I was being “overpaid”, I just lived lean.
My VA claim is 8 years old. I finally got a C&P exam last year and was awarded 50%. My VA psychologist pulled up the new DBQ? form on his computer one week later and said the C&P examiner did not rate me properly. He said I should have been rated higher.
I have a BVA hearing next week on the issue. It’s just so hard for me to understand why VA won’t listen to their own VA psychologists? My claim would fall into the category of ‘improper award’ since it was under-rated.
So, to remedy this, will they start “recouping” their improper payments automatically from veterans deposits for disability? I could totally see this happening, and what could we do about it? Nothing! The VA is starting to look as corrupt as the IRS, and that is scary considering the size of this agency, with obviously no uncorrupted oversight, and the positive or in this case negative influence that they can have on a disabled veteran’s life. And the hits just keep on coming… Very sad… No… Pitiful!
Next?
There will be a ‘story’ about an undeserving disabled vet who gamed the system.
Then,
a ‘story’ about why disability payments should be taxable.
Then,
a ‘story’ about vets who receive disability payments while holding a good paying job.
Read Congressman Jeb Hensarling’s (R-Tx) newsletters. How about your healthcare being taxable? How about a freeze on COLA? How about ‘reining in the spiraling VA costs’? How about a ‘cap’ on income tied to your disability payment?? And, Jeb is not alone — a number of his colleagues are already on record supporting such things.
just sayin
Obviously the DVA’s play on the Veterans momentum towards bringing to light the inadequate way management of the VA has been to Veterans and the American taxpayers who support the Veterans and their deserved benefits. Hopefully this attempt to play head games with the public will back fire on them.
Ben’s post and the comments include many valid and important points. Legislators, especially Congressional Veterans Affairs Committees should read this blog and interview Ben and some of the commenters where feasible. They will learn a lot.
One area that needs much more attention is the low quality and lack of consistency of C&P exams for PTSD and other mental disorders. Way too many fakers and exaggerators receive VA disability benefits, and way too many legitimate claims are denied or under-rated. *Both* types of inaccurate results need to be addressed. Currently, Veterans Service organizations focus on the later, even though every veteran personally knows some fakers and exaggerators.
Joey, nice post. However, I do know some fakers but do believe there are veterans out there who have been over-looked for many reasons. For example, most veterans in which I have served with seem to know everything: especially when they out rank you. You cannot tell them anything (i.e. make sure your 201 files / medical records are up to date before out processing, or file a VA claim before out-processing) because they know everything and find more pride in over-talking those who do know a thing or 2 about the VA system (i.e. former 30 year US Army 1SGT trying to help process an active duty SSG’s claim). Then they wine (i.e. SGTs – SFC) and throw a fit once they hear their fellow soldier counter-parts are getting a better end of the stick.
WE both lack cannot properly speak about those who are getting their benefits because we have no expertise in the VA Claims processing field. Yes, I am disabled and receiving my benefits to include mood disorder medications, prosthetic limbs, etc. If you could see me and if I told you I was getting VA benefits, you would probably eyeball me down to see what was wrong with me even though I look normal (from therapy and training) then make your decision that I was a faker right? In conclusion, life is about covering your 360. Don’t hate on those whom have. The laws are different outside of the military. Veterans have a tenancy to sue others who announce them as: fakers without any valid evidence. Trust me when I say I have seen it and it has not been a pretty picture for the accuser in civil court. No UCMJ only true justice for the fallen and disabled.
Fake? I was once called fake by people like yours Mr. Joey Anderson. I almost believed those who called me fake and thought I might have been reading too much into it until 2 years later after discharge I attempted to commit suicide because of the my divorce, loss of custody of my kids due to the war, and those dam sharp sounds around me remained unbearable at times. Then, I had to admit there was something seriously wrong with me. Now, I am receiving treatment and care through my VA hospital in which I respect because if it weren’t for you accusers motivating me to suck it up then I would be dead. It is the same crap that has been going on across all branches of service whenever a soldier reaches out for treatment. Yes, I get compensation from VA but would give it back to live a normal life before Post 911. So, I guess I have y’all to thank for it right?Good luck obtaining your VA benefits. I hope you receive them and wish you the best of luck. SGT Blum made a good point. IF you are not educated on the issue then leave it to the experts. You know what the say when you A.S.S.U.M.E. (You make an ass out of yourself and your fellow veterans who have served beside you regardless of how much more you think you should receive than that man next to you who got out of details etc.) There is always a reason for everything and eyes who know the real truth (i.e. CID).
SSG Johnson – Yes, some veterans have been accused of faking when they were not. That is the most egregious type of inaccurate exam and examiners, who because of bias, incompetence, or whatever the reason, falsely accuse veterans of faking should be fired.
My point is that such examiners, along with the ones who rubber stamp almost every claim, are rarely identified because the VA does not have an effective quality assurance program for C&P exams.
In the past the VA policies were too strict and rigid about PTSD claims. But the pendulum has swung the other way since the 2010 change in the regulations regarding stressor verification. That chane was a good and important one. But along with it came an emphasis on production (get more claims processed in less time), and a decision to pretend that all mental health C&P exams are accurate, whether completed by VA staff or contractors. Some vets think this is fine because at least more genuine claims will result in service connection and disability benefits compared to the past. However, over time passivity on this issue will mean a lot of fakers, exaggerators, and misattributors will receive undeserved benefits and their will be a public backlash against compensation for PTSD and other mental disorders.
What do I think?….. I think that I am fed up with the attention hogs i see constantly in any news media getting partial Intel and running with it just so people can get in an uproar without knowing ALL the facts. So until I hear more that our government will allow I will reserve my opinions.
I believe in these principles: 1) Accountability Of, 2) Responsibility For and 3) Fair and Just. Doing the Right things the RIGHT WAY NOT the so-called hearsay rules and regulations that has been adopted by the VA and not following the Federal Statutory laws and Regulations. Yes, there are hard working VA employees, but the ones that are at the Top of the food chain should be held Accountable for not being Fair and Just to all that had served this Great Nation of ours. We the People are at fault for letting this situation go from bad to worse because We the People voted for our representatives so the blame is not only on the VA, but everyone.
Then we can get to the meat of the matter and tally up all the illicit, undeserved “Bonuses” to VA management across the board over the past 10 years alone.
And can’t those payments be considered unjust “overpayments” as well, since they were paid out regardless of whether their jobs were well done at all? We would hope so.
And let’s not forget all the taxpayer monies wasted on ridiculous fully paid vacations by thousands of VA employees who got to go to the many VA “training seminars” where they spend most of their time there just screwing off and being entertained. Let’s go back over the past 20 years with that figure. And as our baseline for estimating, let’s use the $9 million blown at the Orlando, Florida “seminar” that came under such heat from the Senate and House VA Committees.
I think if we just take a real hard look at the above figures, we will come something close to several Billion dollars, and maybe over $10 billion that VA pissed right down the drain.
But let’s never, ever consider the total dollar figure that was NEVER paid out to veterans or their families by being shafted by the VA. For that figure, let’s go back over the past 40 years from 1970 to the present. Figuring up that horrendous total would likely call for long prison sentences for the criminals who ran and run the VA — and are responsible for carrying out VA’s “progressive-socialist” plan to dishonor America’s most honorable.
I can categorically assure you that the bonuses, as totally undeserved as some or most may be, are not illicit. If they were, they wouldn’t have gotten them at all. Furthermore, there are a plethora of reasons a person can earn a personal bonus. I know former VA employees who worked in their IT support. Many are extremely good at what they do and I saw a lot of hard, creative, and innovative work done by a couple of them. Even with the current debacles, lots of outstanding support personnel who do their jobs with excellence should not be denied reward for their work nor should they have their reputations besmirched. However, the management and executive level civil servants responsible for the current debacles are totally undeserving and how bonuses got approved for them should get a thorough investigation and the guilty reprimanded.
Just another of the long line of half-witted VA reports that “purport” to tell us something important. But what can you believe from an agency that has a proven history of LYING?
Lets take another perspective and see how those numbers add up: Out of the total claims filed and eventually won on appeal to BVA or CAVC or higher, what is the total dollar amount awarded — and don’t forget to factor in the interest at 10% per annum, which is the rate paid in all civil actions where an appeal had to be taken, and the losing party required to pay the interest accumulation to the total time spent on appeal.
Looked at another way: Let’s take the total dollars finally paid out to veterans and their widows and families after they had to file repeated claims over the span of many years before finally being awarded their just compensation. And don’t forget the mandatory interest accumulation, and compounding during the course of the appeals, or any inexcusable delays due to typical VA incompetence.
Next, lets add up the bonuses awarded to VARO claims adjudicators who met their quota of processing claims cases — whether decided correctly or not — and see what dollar figure we get there for the total rate paid out nationally.
Amen
ALL IS “FAIR”(FARE) IN LOVE AND WAR, BUT WHICH ONE ARE WE DEALING WITH IN THIS INSTANCE.
Comments are closed.