A new GAO report exposes that Veterans Affairs shamefully put veterans lives at risk by failing its duty to report bad doctors and other clinicians.
The GAO report confirms a USA Today report exposing VA has concealed and avoided investigations and mandated reporting of bad health care workers for many years. Maybe if VA had followed its own mandatory reporting guidelines, veterans like Charles Ingram, the veteran who burned himself alive, would still be with us.
GAO Report Exposes Veterans Affairs Bad Doctor Reporting
The GAO report in question evaluated only 5 locations and found VA failed to report 8 of 9 clinicians. Unfortunately, the report fails to tell readers which facilities were evaluated. Obviously, one would expect one star rated facilities like Phoenix VA to have more failures than five star rated facilities like Minneapolis VA.
RELATED: VA Testing PTSD Treatment Using Meditation
Providers at the unnamed facilities were not reported because “officials were generally not familiar with or misinterpreted” the policies.
“At one facility, we found that officials failed to report six providers to the (national database) because the officials were unaware that they had been delegated responsibility for…reporting,” the GAO said.
GAO also found VA failed to maintain adequate documentation on almost half the investigations.
RELATED: Five Veteran Deaths Linked To One VA Medical Center
Per USA Today, “a total of 148 providers required clinical reviews after concerns were raised about their care between October 2013 and March 2017. But in nearly half those cases, the hospitals could not provide documentation that the reviews occurred.”
“We found that all five (hospitals) lacked at least some documentation of the reviews they told us they conducted, and in some cases, the required reviews were not conducted at all,” GAO concluded.
RELATED: VA Goes Hi-Tech With iPad Program
USA Today and other mainstream media left out the specific procedures GOA said VA was supposed to follow. It included it straight from the GAO report italicized below for your review. Veterans should be able to track this to help guide them when reporting wrongdoing by a clinician.
Below are those proceedures and their findings:
Download: GAO Report Bad Doctors
Veterans Affairs Clinician Care Review Requirements And Results
Triggers Requiring VA To Evaluate For Possible Adverse Reporting
As part of the credentialing and privileging process, VAMC officials are responsible for monitoring each provider’s performance on an ongoing basis and identifying any concerns about clinical care that may warrant further review. VAMCs can identify concerns about providers’ clinical care in a variety of ways, including the following:
- Ongoing monitoring. VHA requires VAMCs to conduct and document ongoing monitoring of each provider’s performance at least twice a year through an ongoing professional practice evaluation. During this evaluation, a provider’s performance is evaluated against benchmarks established by VAMC leadership that define acceptable performance, such as documenting patient visits appropriately and achieving specific patient outcomes.
- Peer review triggers. VHA has a separate process, called peer review, that VAMCs may use to review adverse events. While information collected as part of peer review is protected for quality improvement purposes and may not be used to take action against a provider, VAMCs can identify concerns about a provider’s clinical care based on a trend of certain peer review outcomes over a specified period of time, referred to as triggers. VHA requires VAMCs to establish peer review triggers. An example of a peer review trigger is when a provider has two or more episodes of patient care within a 12-month period for which a peer determined that most experienced, competent providers would have managed the episodes differently.
- Complaints or incident reports. Concerns about a provider’s clinical care can also be identified through complaints and incident reports.17 These can come from any individual with a concern, including patients, providers, or VAMC leadership.
- Tort claims. Filed or settled tort claims or malpractice claims can raise a concern about a provider not identified through ongoing monitoring or peer review.
Types Of Review VA Is Supposed To Do (But Won’t)
Once a concern about a provider’s clinical care is identified, VHA policy and guidance establish processes for VAMC officials to use to review the concern and determine whether an action should be taken against the provider’s clinical privileges. VHA policy states that if allowing a provider under review to continue delivering patient care could result in imminent danger to veterans, VAMC officials should remove the provider from delivering patient care through a summary suspension of privileges. VAMC officials have flexibility to determine the most appropriate process to use to review a provider’s clinical care depending on the specific concerns and the situation. These processes include the following:
- Focused professional practice evaluation (FPPE) for cause. This is a prospective review of the provider’s care over a specified period of time, during which the provider has the opportunity to demonstrate improvement in the specific area of concern. Failure to improve could result in further review or action.
- Retrospective review. This is a review of the provider’s delivery of patient care focused on a specific period of time in the past, a specific area of practice, or both, based on an identified concern.
- Comprehensive review. This is a more extensive retrospective review, generally performed by a panel of experts to ensure fairness and objectivity. In addition to reviewing the provider’s past patient care, these reviews may also include interviews with the provider, patients, and staff. These reviews generally result in conclusions about whether care delivered by the provider met the standard of care and may include recommendations about the provider’s privileges.
Steps VA Might Take (But Doesn’t) To Protect Veterans
Once a review is completed, VAMC leadership officials and the VAMC credentialing committee make decisions about next steps, which could include the following:
- Do nothing, if the review did not substantiate the concerns;
- Conduct further review (such as an FPPE for cause to allow the provider an opportunity for improvement or a comprehensive review if more information is needed); or
- Take an adverse privileging action, including limiting one or more privileges (such as prescribing medication or performing a certain procedure) or revoking all of the provider’s privileges.
If the VAMC’s credentialing committee recommends an adverse privileging action, it is the VAMC director’s responsibility to weigh all available information, including recommendations, and take an action. After a permanent provider is notified of the director’s decision, the provider can appeal the decision to the Disciplinary Appeals Board as part of their due process rights. The adverse privileging action is considered final once the Disciplinary Appeals Board reaches a decision and the Deputy Under Secretary for Health executes the Board’s decision. If a permanent provider does not make use of the offered due process procedures within 7 days, the provider waives his or her right to due process and the adverse privileging action is considered final.
Reporting VA Is Required To Follow
VHA policy requires VAMCs to alert certain entities if there are serious concerns with regard to a provider’s clinical performance. VHA policy assigns reporting responsibility and authority to the VAMC director, who generally delegates the task of reporting to other VAMC officials. VHA makes this information available to other health care entities through two distinct reporting processes:
NPDB. Under VHA policy, VAMC directors must report to the NPDB any adverse privileging action the facility takes that 1) affects the clinical privileges of a provider for a period longer than 30 days and 2) is related to professional incompetence or professional misconduct. VHA policy requires VAMCs to submit these NPDB adverse action reports within 15 calendar days of the date the adverse privileging action is made final— that is, when all applicable internal due process procedures have been completed and the VAMC director has signed off on the action. VAMC directors are also required to report to the NPDB providers who resign or retire while under investigation or in return for the VAMC not conducting such an investigation or proceeding. To avoid any errors in the facts of the report, the VAMC director must notify any provider who is about to be reported to the NPDB and give the provider an opportunity to discuss the content of the report before it is submitted.
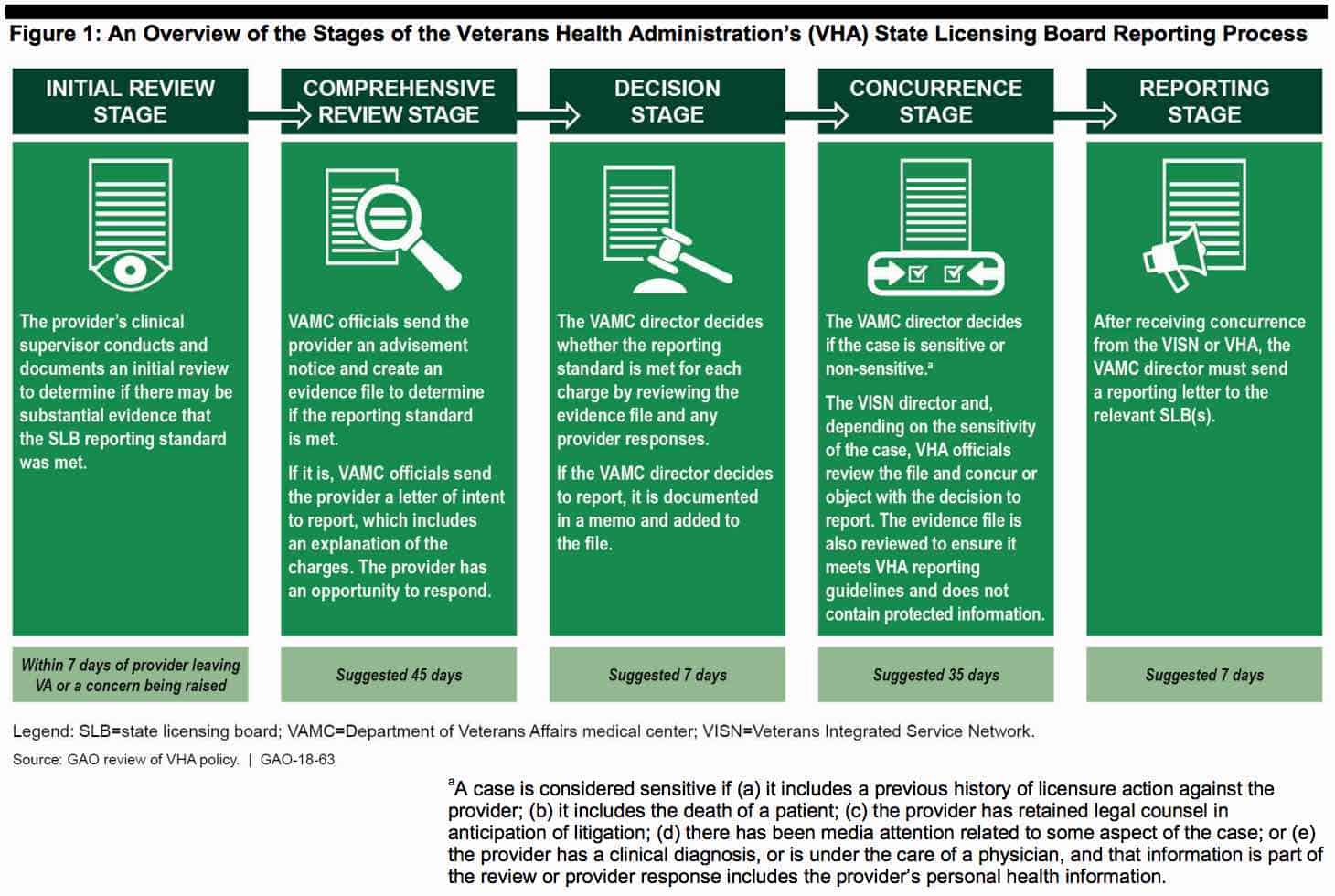
SLBs. VHA policy requires VAMC directors to report providers—both current and former employees—when there are serious concerns about the providers’ clinical care to any SLB where the providers hold an active medical license. Specifically, VHA policy requires VAMCs to report providers who so substantially failed to meet generally accepted standards of clinical practice as to raise reasonable concern for the safety of patients. According to VHA policy and guidance, the SLB reporting process should be initiated as soon as it appears that a provider’s behavior or clinical practice fails to meet accepted standards. VAMC officials are directed not to wait to report to SLBs until adverse privileging actions are taken because an SLB conducts its own investigation of the provider to determine whether licensure action is warranted. This reporting process comprises five stages as established in VHA policy, and VHA policy states that the process should be completed in around 100 days (see figure 1).
Clinical Care Quality May Impact Performance Pay
Performance pay—a component of VA provider compensation—is an annual lump sum payment based on the extent to which an individual provider achieves specific goals. The goals may vary for providers across VA, at the same VAMC, or within a particular specialty. VA policy establishes minimum performance pay eligibility criteria, including being employed by VA from July 1 through September 30 of the fiscal year being reviewed.
Clinical Care Findings
Documentation frequently lacking. We found that the five selected VAMCs collectively required reviews of 148 providers’ clinical care after concerns were raised from October 2013 through March 2017, but VAMC officials were unable to provide documentation that almost half of these reviews were conducted. We found that all five VAMCs lacked at least some documentation of the reviews they told us they conducted, and in some cases the required reviews were not conducted at all. We also found VHA does not adequately oversee these reviews, as discussed later in this report.
- FPPEs for cause. FPPEs for cause accounted for most of the missing documentation of clinical care reviews, despite VHA policy requiring VAMCs to document FPPEs for cause in the providers’ files. Specifically, of the 112 providers for whom the selected VAMCs required FPPEs for cause from October 2013 through March 2017, the VAMCs were unable to provide documentation of the FPPEs for nearly a quarter (26) of the providers. Additionally, VAMC officials confirmed that FPPEs for cause that were required for another 21 providers were never conducted.
- Other reviews. The selected VAMCs were also unable to provide documentation of some retrospective reviews. Specifically, of the 27 providers for whom the selected VAMCs conducted a retrospective review, 8 were missing documentation. While VHA guidance recommends that VAMCs document these reviews, VHA policy does not require that VAMCs document retrospective or comprehensive reviews. VHA officials told us that they expected VAMCs to document these types of reviews so that the information could be used to support adverse privileging actions, if necessary. Without clearly stated documentation requirements in VHA policy, VAMC officials inconsistently document their results, preventing VAMC directors and VISNs from properly evaluating the effectiveness of its retrospective and comprehensive reviews, which are used to, among other things, ensure patient safety. Additionally, we found that key officials from two VAMCs were not aware of the VHA guidance and that 5 of the 8 missing retrospective reviews were from these two VAMCs. We also found that one VAMC was missing documentation of clinical care reviews for 12 providers who met the VAMC’s peer review trigger. In the absence of this documentation, we were unable to identify the type of reviews that were missing for these 12 providers.
The selected VAMCs’ failure to document reviews of providers’ clinical care after concerns were raised is inconsistent with federal internal control standards for monitoring and documentation, which state that management should conduct and document separate evaluations, when necessary. In the absence of VAMC documentation of such separate evaluations of providers, VAMC leadership officials lack key information needed to make decisions about whether providers’ privileges are appropriate, and they also lack reasonable assurance that appropriate reviews are conducted.
Reviews not always timely. We found that the five selected VAMCs’ reviews of providers’ clinical care were not always conducted in a timely manner after concerns were raised. Specifically, of the 148 providers, the VAMCs’ initiation of reviews of 16 providers’ clinical care was delayed by more than 3 months, and in some cases for multiple years, after the concern was raised. At one VAMC, service chiefs were not instructed to conduct reviews of 14 providers until 4 to 13 months after these providers met the VAMC’s peer review trigger. Before the service chiefs were notified of the concerns, 3 of these providers had at least one additional concerning episode of care—that peer reviewers judged would have been handled differently by most experienced providers—identified through the peer review process. As pointed out in VHA guidance, earlier intervention could prevent additional patients from receiving substandard care. Officials from another VAMC did not conduct retrospective reviews on 2 providers until we requested documentation of the reviews, approximately 3 and a half years after the credentialing committee had initially requested a review.
While VHA officials told us that clinical care reviews should be conducted as expeditiously as reasonably possible, VHA policy does not specify a timeliness requirement. Allowing more time to elapse before a clinical care review is initiated weakens the intended purpose behind clinical care reviews and further increases risk to patient safety. Federal internal control standards for monitoring state that management should evaluate issues and remediate identified deficiencies in a timely manner. A clinical care concern could represent a potential deficiency in providing medical care, and as a result, VHA increases its risk further without establishing a policy that sets timeframes for conducting clinical care reviews.
VHA oversight is inadequate. We also found that VHA does not adequately oversee VAMC reviews of providers’ clinical care after concerns have been raised, including ensuring that these reviews are completed and documented in a timely manner. Under VHA policy, VISNs are responsible for overseeing the credentialing and privileging processes at their respective VAMCs. While reviews of providers’ clinical care after concerns are raised are a component of credentialing and privileging, we found that the VISNs with responsibility for overseeing the selected VAMCs through routine audits do not include these reviews in their audits. While the standardized tool VHA requires the VISNs to use for these audits instructs the VISNs to identify and review providers who were on an FPPE for cause, none of the VISN officials we spoke with described any routine oversight of FPPEs or any other reviews of identified clinical care concerns. This may be in part because some VISN officials are not using VHA’s standardized audit tool as required. Officials from one VISN said they had developed their own audit tool and officials from another VISN said that they were not conducting the audits due to multiple instances of turnover in a key position at the VISN. Further, VHA’s standardized audit tool does not direct the VISN to oversee any other types of reviews of clinical care concerns, such as retrospective or comprehensive reviews. The tool also does not require VISN officials to look at documentation of the FPPEs for cause; instead, it calls for reviewing credentialing committee meeting minutes. Without reviewing documentation, VISN officials would be unable to identify the incomplete documentation that we identified in our review. Both VHA and VISN officials described instances of assisting VAMC officials with reviews of providers’ clinical care after concerns had been raised, but VHA and VISN officials told us that their involvement in these reviews is typically consultative and not routine. (For example, the VISN may assist by identifying providers outside of the VAMC to conduct the review.) As a result, VHA and the VISNs are not conducting routine oversight to ensure that VAMC reviews of providers’ clinical care after concerns are raised are conducted appropriately, including adequately ensuring that the reviews are completed and documented in a timely manner, in accordance with VHA policy.
The lack of routine VHA oversight, through the VISNs, of VAMC reviews of providers’ clinical care after concerns are raised is inconsistent with federal internal control standards for monitoring, which state that management should establish and operate monitoring activities. In the absence of routine monitoring of VAMCs’ evaluations of providers after concerns have been raised, VHA lacks reasonable assurance that VAMCs adequately review all identified concerns about providers’ clinical care and take appropriate privileging actions to ensure that VA is providing safe, high quality care for veterans.


92 thoughts on “GAO Report: Veterans Affairs Fails To Report 90% Of Bad Doctors And Other Healthcare Workers”
My question is, where do you go to start the process? I would like to start a complaint and how do I know it’s get to the higher ups and not in the trash.
Could we start a class action? Crimes against humanity? I get every veterans is an individual case, but overall…that’s the issue.
How about we start a change.org to have VA run 24 hours, 365 days a year.
No need to be a whistle-Blower it’s happening in real time.
I told Shinseki and Jeff Miller of this years ago-and most recently POTUS and Secretary Shulkin (and USAToday)
The VA has covered this up for decades as to the NPDB requirements for disciplining doctors .
The “smoking gun” will be “Area 1151″….
I dont use linkedin or facebook so dont know if this will go through.
Berta Simmons Volunteer vets advocate and widow of Rod Simmons, death by VA.
(FTCA/1151)
PS
The WH and the Secretary’s office responded to my last correspondence and I await whatever their (WH)recent email to me involved.
I thought it was about a Fast Letter I wanted the Secretary to issue-and made a good argument for that- but now I think it is about ‘reviewing ‘ in their words
“area 1151″ ….
I will sing like a bird on that.
Deep throat was right….”follow the money”
VA has 700 lawyers to defend or assist in these cover ups. If you do this you can get away with it. Just deny or blame someone else. Oh that happened before we were in charge. Or I forgot. Really there is a regulation that I was to follow.
Just throw the complaint away and they cant prove anything against you. Just Promise you will do better. Regulations are made to be broken. don’t worry we have your back.
Veterans who claim they have been mistreated ! just turn the Table on them and accuse them as being disruptive! problem solved just blame the veterans the public knows all veterans are crazy so don’t worry about any proof we have your back.
But Veterans are dying !!! And your point is what ! Listen if you don’t blame the veterans you will be held accountable and you can loose your job, do you want to loose your Job ?
No ! well do what you need to do and blame the veteran. Don’t call the local police and tell them that the veteran has been Disorderly or they will hire an attorney and have their day in court and you can be found to be making false Reports against the veteran.
That’s why we have the Disruptive committee, don’t worry about making any report trying to justify us punishing the veterans, we will teach those veterans to speak up.
We are the accuser and the Prosecutor and the Judge so the veterans are not able to seek any council or anyone else to help. We are the Justice Department.
So we dont need any proof of the Veterans Actually being disruptive. It would be nice to have something in writing, but its not necassary. I have know you for years, we drink togather, your my childs God father, I have your back. You mean I am a God ! I said God father, so same thing, I guess !
Why not just tell everybody on these veteran’s website what the VA is doing.
For example,
1. Peter M. Barach NPI #1396773610 Ohio, License #3280 Ohio C and P Exam Hatchet Man Aka Dr. Frankenstein, Aka The Monster of Shaker Heights. Wade Park VA Cleveland Ohio. This guys Peter M Barach Jewish Catholic Non Veteran Draft Dodger 1970-1973 is “Cherry Picking” through medical records (6 or t months worth of tainted notes) and creating these 20 page C and P exams and handing them off to DRO (decision review officers ) in cleveland Ohio. This klown Peter M. Barach is lying, falsifying, and manipulation reports (false narratives) with impunity.
2. The Medical Director Susan M Furher Wade Park VA Cleveland Ohio is fully aware of what Peter M. Barach is doing to injured veterans and disabled former soldiers. And so are all Ohio State Reps! Susan M. Furher asst Jeff McPeaks Phone 216-791-3800 Ex 4070 is fully of aware of Peter M Barach inappropriate behavior, unethical conduct and outright lying.
3. So of the hundreds of pages of medical notes, documented injuries in service from private doctors from Ohio. This Peter M Barach is only picking out one Catholic Non Veteran Draft Dodger from Lancaster Pennsylvania. Peter M. Barach is then taking this one doctors tainted 7 months worth of tainted medical records, and thus “Cherry Picking” the bogus sentences from this Catholic Non Veteran doctor, and thus creating these bizarre corrupt adversarial C and P Exams. Then handing it off to these DRO decision review officers in cleveland Ohio.
4. Senator Sherrod Brown Ohio, Senator Rob Portman Ohio, and Congressman Tim Ryan’s Office in Ohio are fully aware of this, and have my complete records with detailed letters, and fully developed claims from private doctors (actually VA approved doctors)…
5. Came in to the Akron Ohio VA with a 1st fully developed claim, DBQ forms filled out by private doctors. This is on record.
Then spent oct 2014 to Feb 2016 with 1. ERIC CANNA Non Veteran Catholic and 2. Pamela Sue Sherer Non Veteran Catholic And soon found out these two were doing some seriously corrupt sh*t to my VA medical notes.
6. SO, I quite left, march of 2016, and obtained a private military doctor, and again. Another fully developed claim (A 2nd fully developed claim) was created by this private expert. MMPI (social history with symptoms of injury), Orgins of Diseased Report (5 pages long), DBQ forensic evidence, and a Nexus letter. And countless letters of legal testimony…
7. And then what this crazy son-of-b*tch, and pr*ck did, PETER M. BARACH C and P hatchet man VA Wade Park Cleveland Ohio making tens-of-thousands, if NOT hundreds-of-thousands of dollards F*CKING disabled former soldiers and injured vets is completely attempt to cover up mal-practice by VA Employees 1. Pamela Sue Sherer, and 2. VA Employee Eric Canna. “An VA Abuse Team!”
PETER M BARACH By creating this bogus 20 page C and P exam, that nobody at the state has ever seen before nor heard of. PETER M. BARACH NPI #1396773610 and License No.3280 Ohio. Still has not been discplined, nor held accountable. For his lying, falsifying medical notes, and attempting to mislead, and discriminating against injured vets and disabled former soldiers. Still Peter M. Barach and his associates at the VA have not been held accountable for their wrong doing.
8. All the while from the summer of 2014 to June 2016 the VSO (Veteran Service Office) caseworker Summit County Ohio is re-filing, re-filing, and re-filing my claims without my permission behind my back. The case worker at the Summit Co VSC (Veteran Service Center) was giving these two time,
1 Eric Canna VA Akron Ohio Waterloo Road Catholic Non Veteran time to build bogus medical notes on me to make up bull sh*t that I was hurt somewhere else. 2. Pamela Sue Sherer VA AKRON OHIO Catholic Non Veteran to create misleading medical notes and bogus disorders
I imagine this is what Chris Attig calls “Develope to Deny” or “Delay to Deny” in the face of overwhelming evidence to grant me my claims.
9. Then PETER M. BARACH picks up these notes, and “Cherry Picks” bogus notes, uses my fully develope claims from private doctors (copies stuff and changes it, lying) and creates this bizarre 20 page C and P exam, lying with imputy in April of 2017. Leaving all favorable evidence of injury in service and disability from service out of this corrupt 20 page C and P exam. This is all explained in great detail to the DRO decision Review officer in May of 2017, and this is all explained in great detail to the Senators Rob Portman Ohio, Sherrod Brown Ohio and Congressman Tim Ryan Ohio.
10. Forwarding my fully developed claim by FAX from Congressman Tim Ryan’s office to VA Director TONY MILONS Cleveland Ohio.
TONY MILONS, Who stated to us VETS in Cleveland Ohio 2015,
“get me your claims. Go out and get your own private doctors. Get your own private medical exams! And get me their information! There are big problems with the VA Hospitals in Ohio. WE know that at the benefits dept.”
11. So my fully developed claims was forward to VA Director TONY MILONS by the Congressman TIM RYAN’s OFFICE. Congressmand Tim Ryan’s asst MATT VADAS forwarded all these private medical documents by FAX to TONY MILON this past summer 2017. But WE still have not heard from TONY MILONS VA DIRECTOR CLEVELAND OHIO.
it doesnt do any good to recognize a problem if there is no remedy provided, as in who can we report a problem to that has the authority and desire to make the necessary changes, one of the biggest problems is they are all in the gov workers union and as everyone knows union membership 101 says you never do or say anything to make another union member look bad, until that changes I doubt anything else will either. Just an example of what I go through is, I have an infection in my knee, I first went to the ER on dec 30 of 2016, they told me it was a callous and every doc I seen after told me the same thing until I ask what I could do to get the callous to stop draining, then they then tell me how dumb I am and that callous’s dont drain, after 11 months half a dozen “doctors” and all the drama, finally last week they tell me my only option is to let them cut it open and let the air dry it out. They refuse to even do a culture to find out what kind of infection it is or try antibiotics. I told them heck no your not going to cause an open wound in the presence of a known unidentified infection and let the inside of my knee dry out. their reply, if you change your mind come back. whadda you do?
What do you do? Put what you just said in a letter. State in the letter that you want to be referred to someone outside the VA using Choice.
Go to the Patient Advocate, give them the letter, tell them you want to be referred to Choice, and ask who you see to get that referral. Tell the Patient Advocate you want a Report of Contact submitted explaining your visit and your request, and that you expect to hear from the VA in 3 days on that referral.
As for a printout of the Report of Contact.
The Report of Contact is an internal VA reporting system like email that is sent to VA management at your hospital, including the director.
If you don’t hear from the VA within 3 days, call your congressman and ask them for help in getting care for an infection you have had for over a year.
That nor anything else functions/worked like that in Indiana. Not for me it hasn’t and did not. FOIA or congress critters will not reply or just ask for access to your files and history for life but that’s about all. Then sit back and wait for more harassment and other assorted stupid stuff that could only come from a discussion with some senator and congressman’s staff knowing what is going on. Been there done that too many times.
It also does no good giving them unlimited access to all our information when some so-called private medical info is leaked and used by local politicians and some activist to try and torment, harass, or let you know just how much info they can get or know about you. Then the fun begins trying to trace it all back to find a source which is impossible to do.
It also does no good to release our files when the problems in part is the VA or contractors deleting online communications and files that were saved on sites like the Healthy E vet thing, which can’t be found again, along with the threats and incompetent nature of it all. Zip…there goes the evidence and same goes for lies and deceit in our files to cover for their abuse to total lacks of concern or corruption. Dealt with the same crap with civilian care covering up for the VA. Mds not wanting or making it difficult to obtain files, refusing to Xray to prove incompetence/damages, finally submitting a phony file, paper, that was not the same one I seen in the doctors office at all, or signed copy of what I had to read and was written done. It’s all a damn game.
I thank you for your suggestions, I did go see the advocate, they are worthless, so I then went straight to admin, pretty sure/hope it will be resolved soon. If I had known about submitting it in writing to the advocate before I sure would have, perhaps that would compel them to act. Again thank you
Ken, depending on how long ago this was, you can still put it in writing.
Address it to the director and hand carry it to their office. State in your letter that you went to the Patient Advocate on XYZ date, but nothing has been done.
You will likely only see the directors executive secretary because the director is passed out under his desk, but do it anyway. Ask the secretary to submit the Report of Contact.
Create that paper trail. Believe me. It may come in handy in the future.
In the last FOIA I received from the VA, it included Reports of Contact I requested to be submitted at times. It proved what I told certain VA officials and the time they were made aware of them.
The VA tried using those Reports of Contact against me in responding to my congressman until I explained to the congressional aide what each contact was about.
It seems you are well versed on this subject and I very much appreciate you taking the time to help, do you know of any laws, or written policies relating to what you have said and if so where I can find them. I do not question that your suggestions are good and I am going to use them, I would very much like to be able to refer to the laws if needed
Ken, the only law involved here is the Freedom of Information Act. You can find good articles here written by Ben that discuss it, and include templates on how to write one. Its submitted to your VAMC FOIA officer, which usually is also the Privacy Officer.
Reports of Contact are essentially an internal VA reporting system that is a report sent to various VA managers like the Chief of Staff and Director alerting them to potential problems, or a vet raising hell about a problem that could rise to a bigger problem such as adverse media coverage.
The Patient Advocates are supposed to help vets with problems, but they have degenerated into lazy slugs that refuse to do their jobs, or outright cover for VA screw-ups. Saying anything to them verbally is often useless. Putting things in writing creates a paper trail they can ignore, but it is a record you can use to show they were informed of a problem. If they refuse to do their job after being informed in writing, you can attach that letter to a letter to the Chief of Staff or to the Director.
If they still refuse to do their jobs, you can use those letters when you contact the VISN director, the IGs office, the Secretary of the VA or your congressman.
You could also refer to them if you called the White House hotline by telling them the dates and times and who you informed at your VA. The hotline does work.
In the current climate, each would have to wonder what might happen if they ignore your letter, and you take those letters to the media.
The VA really does not like bad press, and they will blatantly lie to make excuses, but if you go to the media, you can bet the VA will become very helpful.
Given your situation, I suspect they are ignoring the problem because they screwed up. Whatever it is, I suggest you get it checked out. You don’t want to be like one vet at my VA who lost his leg because the VA ignored an infection.
After my knee replacement surgery, there was a patch of skin the size of my palm on the side of my knee that was swollen and scaly. The VA ignored it until I put in writing that I wanted it checked out since my ortho doc said he didn’t think it was infection, but wasn’t sure.
The VA addressed it by giving me a telemedicine appointment where they took pictures and sent them to a VA doctor in Denver to look at, then prescribed some kind of cortisone cream for it. It only took several months.
If I were you and dealing with an infection for such a long time, I would call the White House hotline. When you get a call from your local VA suddenly being helpful, you can ask why the Patient Advocate ignored your request.
you could throw a dart at a listing of all of them and not fail to detect some. Although I had great results with PA’s
I read where vets complaints can be used for judging VA doctors, usually from Tort transactions. I have had P.E. (pulmonary embolisms) twice, D.V.T. (I believe or blood clots in both legs), blinded in left eye twice including E.R. visit to sew up eye ball, surgically installed pacemaker/defib. When I went on operating table I went out expecting to wake to of had Pulmonary Vein Ablation Surgery to cure Atrial Fibrillation. I had 1 episode of A.F. for about 10 or 12 hours once every 3 to 5 months, VA changed meds from Digoxin to Propafenone, to Tiazac, to Ameodarone, to Metoprolol. Every change it became having episodes closer & closer until they had me on full time A.F. & the last 2 changes I argued strongly with the cardiologist as I felt that is where they were headed. The head doctor decided to install the P.M./Defib. when I was out & did not sign for it. He could of been sued out of the country if he was not a VA doctor, & I could of cried as it took away the possibility of having MRI scans which I needed urgently due to major back problems. Also have a damaged right arm that is very painful injured a year ago when they changed meds & did not warn me & I blacked out, having 5 falls with injuries. Also how I injured the eye ball. This was all directly done by VA doctor medical instructions. And having just moved , living with my son whose family now has to care for me in their home, & resulted in transferring to another primary care system from home care to a Pact Team 5 unit with leading doctor at Longview CBOC Clinic. After seeing him first time & explained about 5 ongoing urgent problems needing care & he did not address one item & had me, a priority one vet, make an appointment for 6 months away. Just saw him for the second time today , he listened to my heart, did some minor reflex tests on legs & did not address but one problem he found somewhere in my records & had me make another appointment in 6 months again. We discussed ‘Veteran’s Choice Program’ & explained there were 2 of them & pushed me to get into the programs for
care !!! I listed my name in websites asking to sign in for possible lawyer interest to pick up your case & I never rec’d one response.
”I read where vets complaints can be used for judging VA doctors, usually from Tort transactions”….yeah right if they report those doctors to the NPDB.
When I won FTCA I asked the OGC attorney why my settlement and the doctors who killed my husband were NOT reported to NPDB, even though the VA and NPDB mandate is quite clear on reporting requirements. The NYS disciplined doctors data bank was not on line ,when I settled, not until years later and their names were not on it.
The OGC attorney ( same one who settled with me) told me there were “so many doctors involved in my husband’s death.” that this is why NPDB was never notified I said , “ISN’T THAT THE POINT OF REPORTING THESE QUACKS TO THE NPDB.”
It really does not matter if one VA doctor or a group of VA doctors decide to malpractice against a vet…or in my case decide to continue malpractice and cover it all up (BUT THEY FAILED)
This problem is due in part to the VA General Counsel’s office or any Regional Counsel who signs off under auspices of the US 0f A ,on a major FTCA cash settlement, yet fails to advise the NPDB properly.That way the negligent VA doctors can continue to practice medicine on other veterans,with no accountability at all…. and possibly harm or kill more vets.
We ,as veterans and survivors of veterans ( I am a widow of a veteran)have the right to demand accountability.
The White House Veteran’s Hot line is now handled by either veterans themselves or those who are able to better direct your issue to someone who can help,since the initial hot line was up.
855-948-2311
just proves the accountability act is fake news
I do believe that until someone takes the position that the VA director should be checked for prior military and a background check done on all staff the VA will continue to be corrupt with doctors and nurses and the good old boy personnel that have been there for years and think they control VA we need to rid the VA of these people now ,Some VA places are at 1 star as is the one in ElPaso,Texas ,and 1 star in Big Springs,Texas so I don’t go to either and until they are fixed they will not see me .
joseph l vega… Mine says It’s a 5 star and it sucks also… They just might be 5 star liars…LOL
I suggest the VA use my rating system instead of the standard 5 stars, mine would be -1- turd, with up to 5 large kernels of corn in it, and -2- turds with up to -5- nuts, or -3- turds with a mixture up to -5- of either nuts or kernels of corn, with the most nuts, being nuts, if you go there for healthcare, or even nuts.
I have reported my previous Provider, for about 10 infractions on my annual physical. I have not heard what is happening for at least two months.
“Hawaii Police Order People With Medical Pot To Surrender Guns To The State”
Nick Givas, Daily Caller, 2:37 PM 11/28/2017
“Hawaiian authorities have asked medical marijuana users to “voluntarily surrender” firearms due to their medicinal status. This may mark the first time a law enforcement entity has moved to confiscate guns from cannabis patients.
Marijuana users in Honolulu are expected to turn over all firearms and ammunition to the state within 30 days of receiving the notice, according to a letter signed by police chief Susan Ballard, reported the website Leafly.
The state’s first medical marijuana dispensary opened in August, but federal law prevents patients who ingest cannabis from owning a firearm.”
“https://dailycaller.com/2017/11/28/hawaii-police-order-people-with-medical-pot-to-surrender-guns-to-the-state/”
Yeah, you always hear on the news about the many pot smokers using firearms to hold-up Hostess Outlet Stores or even going for gusto and shooting-up a Twinkie Factory…WTF?
Meanwhile, the law enforcement bloke will go home and abuse his wife or maybe do some scored smack from an earlier arrest…
i guess that was apart of democracy your parents didn’t tell u about
I wonder IF law enforcement over in Hawaii will try and confiscate weapons out in the Waiania or Makaha areas on Auahu (I’m not sure IF I’m spelling those words correctly)? I do know, when I lived out there the police kinda stayed away. They basically let the “Locals” do their own “crime prevention” – if y’all get my drift! LOL!
Same as some areas on the “big island”, “Maui” and others as well! Cops didn’t really want to screw with a lot of the locals!
that’s because there on an island. if the police is in trouble…. what are they going to canoe for help?
remove the schedule one and u can put bullets back in the gun.
I confirm the information contained in the Daily Caller link that Seymore Klearly posted. It represents a double-whammy for veterans on the island of Oahu.
It will NOT surprise me in the least – – – if we shortly see some adverse street actions in Honolulu as a result of this.
As Namnibor says – – – wait for it.
ABSOLUTELY EVIL!!! I filled a complaint with the Chief of Staff (C.O.S.) at the Cheyenne VA about my provider not being qualified and showed proof of her nearly trying to kill me. After the meeting, she was fired. VERY rare incident. This information divulged in this article proves exactly why my complaints were never taken seriously and ignored. The C.O.S. may be a good person but the support staff are the questionable ones. DO AWAY WITH THE GODDAMN UNION!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!! please
well there going to have to. Anyone that now has due process rights, a smart lawyers and that are processed by any union working for a third party is in for some serious lawsuits . due process and the union dont get along constitutionally .
Damn I hate the VA. The sad part is that the Department of Justice defends these doctors and assists in covering their GROSS negligence. Makes me sick to my stomach.
SPOT ON VET1!!!!!!!!
can always vomit on a VA doctor
I find it interesting that on the one hand, as a part of official VA policy, it states the VA can report quacks to State Licensing Boards, while on the other hand, states and the VA claim that states have no jurisdiction.
Which is it? Either states have jurisdiction or they don’t. Who is pushing the bullshit lie that states don’t have jurisdiction? Lazy bureaucrats in the VA? Lazy bureaucrats at the state? Or both?
My experience when I needed to utilize State safety net services for 3 years and having to be re-reviewed every 3-6 months was that State Workers, namely Job & Fam Svcs., Medicaid; were as lazy and listless as VA employees (Federal)…and my experience in that same time with SSA office was *only* marginally better, meaning “LaSquishYa” warming a really large chair at SSA had marginally better 5 inch claws on her hands that made her typing skills only marginally worse than all the other swamp creatures, State or Federal…must be a HELL of a physics experiment Beta-Testing office chairs and deckchairs that need-not be bolted down due to “LaSquishYa” terminal velocity combined with gravitational ass waves.
Lazy begets lazy is what I was attempting there…whether Fed or State, they are both feral.
when your black with no reparations you become lazy. thats how ancestral slavery works
@ted- *NOWHERE* did I even remotely hint at any racial issues, YOU attempted to make it so, or sufficiently expressed, and I say regardless of socioeconomic, racial background, the State and Fed workers in those areas, incl. the VA are lazy or lackadaisical, at best.
Take your race bait and shove it.
you hinted a cultural difference by referencing 5 inch claws on her hand as a statement of racial biasing . that is baiting itself. hey am just pointing out your baiting.
don’t get froggy and blame your baiting on someone else .using terms of endearment by reparations is no way racist itself sir.i do believe black people deserve reparations and social security and government jobs for themselves from what they went through . its the democracy of karma.
remember, your disabled u have no room to explain your peers so don’t use it as an excuse for your hostility. if u do the VA will recognize your improvement and reduce your monetary benefits.lol
your a commentator by someone else’s political gain not a commentator by empathy . show me in action what steps to prepare yourself from malice of government control and i will show u my militia of my people.
u have showed sharing extreme prejudice by your words towards federal employee’s .your already shoving yourself in a hole greater than a young disabled veteran like myself.
Apologies for aggression, but my use of phrase “5 inch claws” has absolutely no racial bias…and I refuse to tip-toe through those looking for political correctness IED’s…it’s getting way out of hand…some people are simple looking to fight. Not me. But taking a person’s words out of context is on you…
Ted, your reply is shockingly ignorant and racist itself. Ignorant because you believe blacks should be given government jobs as some kind of reparation, and racist because you automatically assume 5 inch claws are only worn by blacks.
I’ve seen them on various people, and my sole concern is how accurate their typing is when they are typing something about my health into their computer. I don’t want mistakes made because some damn fool thinks she needs talons glued on and hits 3 keys at once.
As for reparations, would you offer the same to descendants of those killed fighting to free slaves? Or are they just SOL? There is enough of the bullshit you suggest going on already in federal government to the point where disabled veterans of any color are passed over for a job because somebody helped out a sistah. I have seen it happen.
What do you say to the black person, or any other minority that has worked hard to get to where they are based on merit, and they are passed over for someone else using your idea of reparations?
Would it bother you that people thought you got your job not based on competence and merit?
If someone is doing surgery, taking my blood, giving me medicine or flying my plane, I prefer they be competent and not in their job because of some fucked up idea of reparations.
With the VA Tele Med system no one will be able to report a bad VA doctor to their State Licensing board. Instead you may be able to report them in the state they are broadcasting from and since the person reporting the bad doctor is not a resident their complaint will likely go uninvestigated or fully processed.
No actions will be taken with the exception of the person reporting the bad doctor will be placed on the VA’s shit list.
Good point. I can’t imagine either a state or VA investigator getting too excited about investigating a telemedicine appointment.
Or the VA sets up a telemed center off shore where nobody accepts responsibility.
My answer to “reporting” would be done directly WHILE having a VA Telemedicine Hack online live, from wherever the F*^*k they are, but with a camera, I will promptly take a dump, pick it up and do my very best dancing monkey imitation and give it a happy ending with my flinging my poo dump into their suggestion box…that split second will be worth spending rest of days rocking back and forth in straight jacket, laughing maniacally…
theres always urine bag swating also
🙁 this sucks
its a vice versa because there is no procedure implementing how or what document to report such matters to a congregation of peers. meaning there is no stick that separates beating around the bush
This explains a lot to me !!! ENT Doctor can’t cure you so he makes false statements in my file and has some of his buds help him . I have the documented proof and they still would not correct the problem ! They just covered it up more ! One ER Doctor, 1 ENT Doctor and the so called goon squad . But the cover up goes on .
If you can, either ask for a choice referral or use private insurance. If a second opinion contradicts the VA’s doc statement I’m not gonna be happy,
ENT docs are useless at the VA and are expensive. They are not up to current procedures like a ENT doc that specializes in facial reconstruction.
You know a VA ENT doc would not know how to handle the silver colloid molds placed on a persons face after an IED blast nor will the nurses.
I had a nurse at the VA that couldnt name the nasal forceps, but was in charge of the entire Specialty clinic.
Very good, thorough article Ben.
Gee. I’m so shocked. Another VA policy that VA managers don’t follow. As long as there is no teeth to not following a mandatory policy, the incompetence continues. Seems simple. Don’t follow policy, you’re fired. I bet every one of these managers knows who to call if there is a problem with their paycheck.
One has to wonder how these VA and VISN directors can percolate in the VA for years and not be aware of this policy. States have mandatory reporting requirements. Do these directors think they are special?
The policy itself has enough weasel words throughout that even if followed, it still leaves enough room to continue allowing third world quacks to keep working. Words like “reasonable concern”, “imminent danger” and “serious concerns”.
So unless a VA quack is holding a scalpel over the jugular of a vet, the vet is not in imminent danger?
You can bet your life though that the policy on performance pay is followed to the letter and in a timely manner.
If Tort claims are a trigger, one would think after all of the Torts filed in the past 3 years that someone would notice the policy wasn’t being followed.
Those most interesting thing about this is seeing that the Deputy Undersecretary is involved in this process, which suggests Shulkin should be intimately familiar with what a disaster this is. The period studied is 2014-2017. He was warming the Undersecretary chair during that period. Why is this process such a mess?
I also find it interesting that the VA should be reporting issues to State Licensing Boards without waiting for their own internal bureaucratic process to be complete. Any guesses on how many reports have been made during the same period?
I really like the VA showing their iCare motto here though. They say they will have this fixed in a year. It takes that long to educate directors on following policy?
Why not email each of them with the policy attached saying from this day forward, the attached policy is followed or you’re fired? They could fix it in a day.
How many vets will be endangered while the VA continues to fuck around for another year asking their directors to pretty please follow policy?
union procedures always dominate state procedures therefore its not what they dont follow but what other hidden protocol agendas they do follow.find out what hidden protocol agendas they do follow without a conflict of interest from OIG and u will have another scandal exposed.
How can this surprise anyone!!? Government agency’s are completely self serving…. to much paperwork and bad publicity….???
Performance pay—a component of VA provider compensation—is an annual lump sum payment based on the extent to which an individual provider achieves specific goals.
These goals being to deny Veterans their due benefits, credentialing unqualified surgeons to murder Veterans, and an entire host of other BS.
Underlying accelerator? The bonus or “performance pay”, get rid of the incentive, and the incentive to do wrong goes away with it. Of course then your only left with wrongdoings, or incompetence due to actual incompetence, and NOT deviate behavior for pay.
Funny how they “forget” to report anything to do with them, but never “forget” to put in a Veterans record, any and all information detrimental to the Veteran, and only, “forget” to add those decisions that could “help”
╭┳━┳┳━━━━━╭┫╰╮┈┈┈…┏━╮╭━┓┈╭━━━━╮
┃┃╭╯╰╮┈VA┈┃▎▃╰╮.┈┈┃┏┗┛┓┃╭┫AFGE┃
╯┣╯┈╭╯CASH╰╭╯╭▌┈┈╰┓▋▋┏╯╯╰━━━━╯
╱┃┈┈╰╮COW╮┈╰┳┻╯┈╭━┻╮╲┗━━━━╮╭╮┈
╱┃┏┳┳┻┻━┓┣┳┳╯╱╱.┈┃▎▎┃╲╲╲╲╲╲┣━╯┈
╱┃┃┃┃╱╱╱┃┃┃┃╱╱..┈.╰━┳┻▅╯╲╲╲╲┃┈┈┈
╱┗┛┗┛╱╱╱┗┛┗┛╱╱ ..┈┈┈╰━┳┓┏┳┓┏╯┈┈┈
…………………….. ┈┈┈┈┈┗┻┛┗┻┛┈┈┈┈
Fuck you VA/AFGE/SES………..Fuck you very much………..and shit.
Incompetent physicians are shielded by va hospital leadership, particularly in hard to fill specialties. I had a gastro doc tell me my gastro pain was all in my head. He didn’t order any tests either. He did wear glasses but I didn’t get the impression that they were X-ray glasses. After months of pain I’m going to see a real doctor in the private sector,
instead of talking about it writing about it why dont u take action for the press to have no choice but to bring the media involved.
Beware of VA employees in labcoats. The VA and OIG will deny you under FOIA attorney’s license numbers.
The New York licences board said they do not have jurisdiction over federal employees.
Delaware said the same thing.
When I called them on it, all of a sudden they through together a fake investigation.
The State of Colorado initially told me that any medical provider practicing in the state must follow a specific state law in order to practice. The law must be complied with within 30 days of starting practice, or the provider could be charged with a felony.
Some VA providers follow the law, others don’t.
A phone call back to the same State office a few days later and I was told the State has no jurisdiction.
I bet they find they have jurisdiction if the heat is turned up on them.
so who do u contact in this case
Believe me, I have sent the information to a number of people, including several in the media. The info contains links to all of the data, names, the law they are violating, etc., so it can he verified by clicking a few links, and nobody is interested.
Again, only the media could force a review, or a congressman, if only they took enough interest to verify the data.
Perhaps the state would show more interest if I sent them a copy of this VA policy showing they do have jurisdiction, but I doubt it.
I suspect other states have similar laws, but also ignore the VA thinking they have no jurisdiction.
can u send me a link out here in Nevada. reno the worst va out there.
Ted, every state is different. You have to search to find Nevada’s medical licensing boards web site. They have a long list of disciplinary actions taken against medical providers with details of the action taken.
Go to the Reno VAs web site and find their list of providers. That list will provide many, but not all providers working at Reno. Do a web search on their full name to find which state they are licensed in. Go to that states licensing web site to see if there are any disciplinary actions against them.
VA providers must be licensed in some state, but they are not required to be licensed in the state they are practicing in.
If the Reno VA has a provider working at Reno named Dr. Harry Bigknuckles, do a web search on his name. You should find enough history to find which state licensed him. If he is licensed in Florida, you will have to go to Florida’s site to see if any disciplinary action has been taken.
Be aware, just because no disciplinary action is shown on some web site does not mean a VA doctor is competent. It just means that there is no formal documentation of how incompetent they are, or they have not been caught yet, or a state is too lazy to oversee those they license.
Not all states require that information be made public.
I found 17 at my VA violating state law, and at least 4 who had been successfully sued for malpractice more than once.
I also found 2 or 3 practicing with expired licenses.
Try calling the White House VA Complaint Hot Line 1-855-948-2311. According to today.
1. From what a white house staff member explained to me today. Each vet who files an individual complaints, gets a complaint case number now. This is new. Immediately the case number is given to the vet by the white house hot line. And the complaint is read back to the veteran in order to make sure they got the complaint right. They want the VA employees (abusers) name (s). For real!
2. From my understanding, hundreds-of-thousands of Veterans have called the white house hot line number and filed complaints, since the White House hot line was started late this past summer. The White House hot line is finding out. We veterans are telling the truth, about 100% of the time. The complaints filed on the VA and it employees have been overwhelming.
3. The White House complaint hot line has now evolved since late last summer because there have been SO many complaints. The White House complaint hot line has now created a computer program (quanitative program and qualatative program) to keep track of all complaints in the system. And individual employees. *From understanding this program is working just like SPSS (stat program for the social scientist) does for sociologists and behavioral scientist in research in the academia (universities).
4. This white house program should be able to crutch qualitative analysis (information), and quantative analysis (stats) on those abusive VA employees. Through the computer program, the staff hot line is finding out there are complaints against the same VA employees, by many, many “different” vets. This was not known before!
The VA hospitals are not keeping records (Against their fellow VA abusers, in their VA pedophile like ring). The VA hospitals are NOT keeping complaints by the vets nor is the local VA hospitals keeping complaints on their VA fellow employees. No records of complaints, no discpline. This is what the white house hot line is finding out.
5. SO, the program at the White house is now keeping track of bad VA employees where the complaints had vanished in the past at the VA Hospitals. At the VA Hospitals the complaints are vanishing. So the VA employee abuser can now officially be documented by this program. This is what is happening now when you call the VA White House Complaint Hot Line 1-855-948-2311.
6. These articles that Ben Krause has written in the past month of November 2017 are right on target and really hit home with what is happening at the VA Hospitals here in Ohio. The VA is violating your rights. right to due process. Delaying to deny, and developing to deny as Chris Attig explains. The VA employees are committing illegal acts (discriminating agianst vets, violating federal civil rights laws), and engaging in abuses against vets, that almost can not be calculated.
7. Re-read Mr. Krause articles this month, sit down, and think about what the VA has done to you in the past. Put your thoughts on paper. Collect your thoughts! And then call the white house complaint number, and file another complaint. File as many complaints as you want. It is your right as a vet. dont be shy! Name the employee (s)! Let the white house worker read your complaint back to you. Get a case number of that complaint. Chances are there might be another dozen veterans out there that had complained about the same VA employee (s), you had been hurt by…
Yes, the WH hotline works. I called it a couple months ago and got a complaint number. Within 2 weeks, I got a call from my local VA who specifically stated it was about my hotline complaint.
It was about me being contacted by a Choice provider who had not been paid. They were threatening to give the bill to collections.
I provided the details to the VA who said they would contact that provider and get them paid.
I have heard from neither the VA or the provider since.
The VA Patient Advocates, if they worked for the veteran, would assist you in filing reports of bad performance, but they are only there, IMO, to warn the VA of bad behavior so it can be covered up. I had tried to get assistance, but when I went to the VISN about my local Patient Advocates I was quickly ignored by the PA and the VISN that has oversight.
I also, I truly think they form a working or friendship bond because they work on the same property here . That should be a No No !
VA Patient Advocate: Official Job Title: Federal “Company Man/VA rapist” position 50K to 60k to start.
Again the VA is not so much like the “Mafia” as it is more like “a pedophila ring”. Even in the mob, there was a certain level of respect, and honor. And I never recall reading about the mob (Mafia) harming vulnerable citizens, or the disabled. And certainly I don’t recall ever reading about the mob (mafia) harming injured vets and disabled former soldiers!
However, these VA non veteran catholics employees (socialized very well to protect each other from little on up), VA employee draft dodgers, and non veteran Jewish VA employees in Cleveland Ohio at the VA engage in hurting veterans and disable former soldiers with impunity.
“The VA Pedophila Ring”: It is almost like these VA employees are gang banging the disabled vets, or gang raping the injured former soldiers, and thus helping each other cover-up the abuse, just like catholic priest do with other catholic priest’s who are pedophiles, and catholic elders in the catholic church, who protect the molestors in the that catholic church.
The VA Patient Advocate just cover up abuse. The VA Patient Advocate here at the VA Akron Ohio Clinic Waterloo Road reminded me more of Employee Advocates, or an Union Rep. Or a high ranking corrupt Catholic Bishop who protects his molestors and protect his pedophiles in his social networks. The VA Patient Advocates/Employee Advocates are there simply to protect the hospital and their colleagues. Cover up mal-practice. Mistreatment of Vets, intentional misdiagnosis, and lack of documentation of symptoms. And by all means, deny the injured vets and disabled former soldiers every penny they earned and are entitled to.
Think about it. If the patient advocates were truely there to help you. The VA patient advocates would help the injured vet or disabled former soldier by assisting the Vet in filing a formal complaint against the abuser (give the vet a copy of the complaint), give them a complaint number, shoot the formal complaint up the chain of command, and to their sentors and congressman (keeping them posted) and thus get back to the vet in a reasonable amount of time about the abuser (VA employee). None of this is happening. Instead, these VA employees and the VA patient advocate acts similar to what a “Pedophila Ring” would do…
This is not happening at all at the VA Hospitals in Ohio. At least this did not happen in the cases where I had gone to the VA Patient Advocate at the VA Akron Ohio Clinic on Waterloo Road. My complaints still sit there at the VA Akron Ohio, and now those formal complaints have been forwarded to and in the hands of Senator Sherrod Brown Ohio, senator Rob Portman Ohio and Congressman Tim Ryan Ohio. It was worthless to go to the patient advocate at the VA Akron Ohio. Just another person walking around with high heels on, and a dress stealing 50 to 70K in federal money off of those disabled former soldier and injured veterans, who sever had made great sacrifices…
It’s all the same thing in Indiana. Total mafia and activist styled, networking, politically, media, medical boards, and VA sanctioned corruption and cover-ups. That is until some fool goes too public and is caught.
One caught, exposed, out of multitudes of wrongs and mistreatment of veterans who have zero voice due to all the special interest groups and butt kissers.
“https://www.foxnews.com/health/2017/11/26/indiana-night-nurse-says-white-women-raising-sons-who-are-rapists-and-killers-sparking-probe.html”
It’s really rampant here, hating white people and veterans, lefty whites joining in all fun, retaliation, threats, harassment, but people don’t care. You have to play the silent PC game or become a target for every imaginable form of harassment and attacks they can think of. Even after my calling a major local hospital’s administration here I am still getting countless harassing phone calls per day with their numbers and hospital ID on my answering machine. I get them from the local physicians clinic also attached to the same hospital only to later hear I have picked the wrong and worse doctors in town to deal with and whose staff constantly and obviously, intentional, cause me grief just as much as the incompetent VA
did. Just my friggin luck. They will repeat what pharmacy to use for example, I will tell them again, only time and time again they seem to send me to a pharmacy farther away and not the ones I have told them to use, or is supposed to be on file. This is non-stop BS. Again just one small example.
Having a female, black, with four inch long fingernails so long during blood draw she couldn’t get the gloves on to fit or poked through. Yeah, I stayed silent because like other times I was followed around by a staff member to see if I was going to complain or not. To be told later by another staff member that it was smart not mentioning it at the time or as with other issues akin to that or I’d be the one up on racist issues and folder flagged then up for being disruptive, trouble making, or uncooperative.
I can’t anything done in this state or locally about any form of threats or harassment, period. Nothing. Pretty damn sad days when those in the medical field, among many other “Professionals” can get by harassing people, threatening us, trying to silence our grievances in any way possible and get by with it. In or out of the damned VA. Carrying on with VA threats etc. Local colleges and med schools are pouring these activist health care workers out by the dozens to get work at the VA, interning
locally, or deep seated in local politics and in all the local medical fields. I have been shown time and time again, I do NOT live in America any
longer. No representation, no voice, no recourse of actions, no common decency, zero true professionalism or oath keepers. Not in Indiana, just plenty of facade and censoring, oh and plenty of attacks. More like China, the USSR, or N Korea.
T.
The Professional Mafia, but they operate much more like “a pedophila ring”.
I am sorry to hear about that. It sounds like the Ohio VA, and those institutions in South Central Pennsylvania.
1. So many lefties (quit haters of veterans, and former soldiers), and many, many more non veterans, non veteran catholics, and Jewish Non veterans.
Never been prejudice but every professional institution, state funded, and federally funded these individuals worked at (Leftist, Non veteran catholic, Jewish Non Veterans, and non veterans), and ran the places. Sadly this is true in my experiences. Completely controlled the places. Any institution where there were salary jobs, and govt money comeing in!
Hostile enviroments for a veteran! There was “NO” “Veteran’s Preference”. Veteran’s status only identified you (ME) to be targeted for harassment and seemingly discrete discrimination campaigns, and mobbing campaigns to be eventually run out, forced out, and, or fired for some non sense…
2. Every institution I worked and experienced at in South Central Pennsylvania where gov’t salary jobs where to be had. They (Non Veteran, Catholics, Jewish Non veterans) controlled who came and who went, and who was to be kept on forever. They ran the human resources offices. Being an injured veteran, it was impossible to co-exist with these diseased animals. They were always at you at an injured veteran! harassing you, and discriminating against you (mobbing an injured veteran, group harassing an injured vet).
Now it is no different at the VA in Ohio. The same people are employeed at the VA in Ohio, and can not be fired. Doing the same things to us disabled former soldiers like myself, and injured veterans like myself.
3. Every professionals institution where govt money, or state funds were to be had, the supervisors, the deans, community college teachers, and the bosses, and while any full time position at any job where an individual couldnt be fired these employees were Non Veterans, Catholic non veterans, Draft dodgers, or Jewish Non veterans. For the most part! Controlling the institutions fed by govt money, state money, and federal funds…
4. Now the same thing at the Ohio VA. MyVA they say? These individuals control (Leftist, Non veteran Catholics, Draft dodgers, Jewish Non Veterans, and Non Veterans) the VA in Ohio Nobody can be fired. No employee at the VA in Ohio is being held accountable. And who is working at the VA in Ohio, non-veterans, Catholic Non Veterans, Jewish non Veterans and draft dodger veteran haters). Again, the Professional Mafia, that operates more like a pedophile ring…
5. Now who meets me an injured vet and disabled former soldier at the door of the VA Akron Ohio Waterloo Road.
1. Eric Canna Akron Ohio VA clinic Catholic Non Veteran who stated, “ALL VETERANS ARE LIARS. ALL VETERANS WANT IS CARS AND HOUSES. ALL VETERANS WANT IS MONEY. ARE YOU SURE YOU WANT TO DO THAT? WELL THIS WILL EFFECT YOUR VA BENEFITS!”
2. Pamela Sue Sherer Akron Ohio VA Clinic Catholic Non Veteran Waterloo Road Akron Ohio VA Clinic.
6. Soon as they met me at the Akron Ohio VA Waterloo Road door the cover-up in my VA medical notes started. The lies started, and malpractice stated! The omitting of the fact, that i was denied treatment from the VA for years. The lies and sabotage of my benefits for being an injured veteran, and disabled former soldier started. I am discriminated against!
7. With countless medical notes verifying my injuries in service through numerous private doctors and private health professionals!
PETER M BARACH Wade Park VA Cleveland OHIO Pick up my claim strangely: And who lies and manipulates a 20 page C and P Exam in the face of overwhelming evidence, and only uses and “Cherry Picks” from a Non Veteran Catholic Draft dodgers notes who I only seen for 6 or 7 months back in Pennsylvania…Well PETER M BARACH Wade Park Cleveland Ohio.
8. Who lies about injury in service and creates a 20 page C and P Exam false narrative, which is filled with lies at the Wade Park Cleveland Ohio Louis Stokes Clinic but Jewish Catholic Non Veteran Draft dodger, PETER M BARACH NPI #1396773610 License No 3280 Ohio. Absolute discrimination! And still they are NOT being held accountable for their unethical behavior, discrimination, and clear mal practice, and absolute lying!!!
9. Senator Sherrod Brown Ohio, Senator Rob Portman Ohio, and Congressman Tim Ryan Ohio have a complete records of this sickness, identifying them these VA employees in Ohio. Still nothing has been done to
1. PETER M. BARACH Non veteran Jewish Draft Dodger Shaker Heights Cleveland, C and P Exam Hatchet Man Aka Dr. Frankenstein, Aka “The Monster of Shaker Heights”
2. Eric Canna Catholic Non Veteran Akron Ohio VA
3. Pamela Sue Sherer Catholic Non Veteran Akron Ohio VA Clinic Waterloo Road
10. Still these diseased animals with their social support networks are not being fired, nor held accountable…
And who is the injured veteran I asked? “ME!” And who’s VA is this??? “MYVA!”
It all goes to show what kind of country, medical systems, and government/mafias/cliques we are forced to live under, or in/with today. It really is absolutely heart-breaking to know its all so wide spread nationally, vast, and deep it all is. While for one reason or another some elements of the problems are never to be mentioned but given passes to harm anyone who isn’t part of their own agendas or groups. The severe changing of our culture, society, the chronic censoring to book and news banning is beyond horrific and totally pathetic.
Try to have a nice day and thanks for sharing.
Va patient advocates more like brag cadets.
OFF-TOPIC but gravely important: Facebook just announced they soon will be updating their software to “recognize suicidal tendencies through the predictive software, using a person’s posts, words, tense, and context and frequency of posts to automatically alert/forewarn local and federal law enforcement SO THEY CAN INTERVENE”…WTF, Big Brother? And people may wonder why I never got onboard with Facebook, well, there you go…and the VA will somehow worm their way into this to make it easier for the Disruptive Behavior Committee to…intervene…wait for it…
“https://www.disabledveterans.org/2017/04/13/veterans-affairs-launches-new-suicide-prediction-tool/”
“https://fortune.com/2017/11/27/facebook-ai-artificial-intelligence-suicide-prevention/”
Don’t accept jurisdiction of VA and have a magistrate or judge certify jurisdiction if you are detained under false allegations.
more like a congress vote to get a judge to do anything with the va. congress has the vote for it before any judge swings that gavel.monkey see monkey do
[Artificial Intelligence]:
The most basic of requirements to work at the VA.
[Predictive Software]:
Still waiting!!!!!
facebook is a monitoring system for the NSA and CIA now. its a freebie for the US government to compound intelligence information on certain criteria without amending allegation set by post,text or any form of written communications. meaning its there to shut up vets that are suicidal.
You’ve got it ass-backwards or have consumed the “movie version”…facebook actually was and is a direct brainchild of NSA/CIA/BELL LABS and good ol’ IBM and Zuckerburg simply made good packaging, marketed, made it appear to be a public domain thingy…whenALL ALONG FB was Big Brother inviting himself by you all allowing it…
can i see the information or documentation on what you are talking about.
I doubt anyone could prove it was a CIA, ect. initiated program, even if they could its kinda a mute point, what does matter is what they are doing with it now and it dont look good but I doubt it could be any worse than the false information in most vets medical records, by records I dont mean that phony/sanitized stuff they give you, there is a ton of information in your records that is kept from you ever seeing it
Again we see [“UNNAMED”] VHA’s breaking the rules by making up their own rules!
I also believe, and agree, IF these “reprobates” called healthcare providers had been FIRED, veterans would STILL be alive!
I’m also of the opinion, the directors of VHA’s won’t do their jobs: Because, IF the truth were to get out, there would be a greater push to “CLOSE DOWN THE VA!”
This is kinda like when someone in Congress commits sexual misconduct and then “bribes their accuser” into “NOT filing criminal charges! This is accomplished by paying the accuser with taxpayers monies. Monies which comes from a “Slush Fund” Congress set-up back when Clinton was in office! Oh, did I forget to mention, the Members’, and accusers’, names are NEVER revealed, just like in this GAO report on VHA’s!
I have noticed, there’s more negative information coming out from other government agencies, on the VA, than was previously reported in the past few administrations! Yet, I don’t see any “corrective measures being taken” against those who commit felonies! It seems as though, they’re STILL wanting “business as usual” in all VHA’s! That’s is: keep poor performance employees and reward them for their poor performances!
Then, fire those who report the poor performers! Basically, telling the “General Population” everything is fine and dandy on healthcare for veterans!
well be the first elf to do something so drastic your reported by all news media accounts that congress has no choice but to shutdown the VA until its fix. if hurricanes can set ratings at 564,000,000 margin from the media. well its time a crazy elf sets the record margin rating. create a bigger hurricane in the va, see what u can come up with.
1) This confirms that 8 out of 9 VA hacks wouldn’t have even been useful on ‘Gilligan’s Island’ as the ‘Professor’s bumbling assistant’, meaning I would trust ‘Gilligan’ performing surgery over the other 8.
2) 8 shitty hacks out of 9 also confirms the VA simply does not give a ratty rat’s ass.
The same goes for VA lawyers with the exception of GI Birch and OIG jack off in conference room king.
There has been absolutely no recourse for those DBC committees that are convened and violate veterans rights.
It goes to show you that veterans lives do not matter when it comes to enforcement of 42 241 and 242.
The DBC is a criminal conspiracy rackeet because the sorry ass Department of Justice wont do their job.
Then when all hell breaks loose, DOJ and VA hide from camera when comfronted with the issues.
Today’s word of the day is #TheHelmanShuffle
Definition: When you feel like a girl name Sharon, but you don’t why, but your titties hurt for no reason and you have just been appointed Secretary of the Department of Veteran Adversaries.
You then are subsequently confronted with life altering decisions for Americas brave men and women, but you run away like Forrest Gump.
Yeah…………………#TheHelmanShuffle
Does “TheHelmanShuffle” cause so much chaffing friction that it smells like bacon simmering between corduroy or Kevlar? 😀
More like “The Mackerel Rena”
Sister of the Macarena
“Heeeyyy Mackeral Rena”! Allriitte!
****Warning****
Those are official DBC phrases should your friendly neighborhood tunabeast walks by at any VA facility.
I was stationed at a Naval/USAF Base in Iceland for 1 1/2 years and the residents of Keflavik, just outside of base, would hang massive amounts of ocean white fish for drying, a fish jerky of sorts, and the smell must have approached what a “Mackerel Rena” reunion festival (or any folk festival).
#TheHelmanShuffle fits right in with the #HokeyPokey that the VA has had veterans dancing to for decades. VA COULD help veterans, but WON’T.
There is ALWAYS a BULLSHIT EXCUSE from these reprobates whenever ANY investigation is conducted. Only way things will ever change for the better is to disband the whole sorry-ass system – – – and begin to rebuild it from the ground up.
How can that be done?
1. IMMEDIATELY recognize the problems inherent in the VA are SYSTEM-WIDE, not just limited to a few locations.
2. Fire all the Lazy No Good Workers. Fire EVERY single AFGE/SES Employee.
3. Sell off all the VA facilities. Alternatively, they may be converted into housing for homeless veterans.
4. Issue all veterans a card that allows them to choose their own doctors within their community that they can TRUST.
5. The United States Government will PAY those doctors promptly (Within 45 days) for the care they provide veterans.
6. ELIMINATE the “Federal Protection” Umbrella for incompetent QUACKS that the VA sends to other states to practice other than their own. Going to practice in Hawaii? You need to be LICENSED in Hawaii. Same applies to all other states.
7. Any claim a veteran submits to the VBA that requires more than 90 days to adjudicate, is automatically found to be in favor of the veteran. If a VBA claim filed by a veteran is found to be a false one designed to scam the system, the VA will have to prove in civil court that a false claim was intentionally submitted.
8. All veterans will be allowed to seek/retain the services of a Veterans Rights Attorney from their first initial contact with the VA.
9. No AFGE, nor any other Labor Union business will be allowed to take place in any Federal Workplace. Conducting Union Business during working hours will be STRICTLY PROHIBITED, and will be STRICTLY ENFORCED.
Should any government employee be found violating this provision, it will result in IMMEDIATE LIFETIME DISMISSAL FROM ANY/ALL GOVERNMENTAL EMPLOYMENT.
10. Attorneys for appeal will be retained at the former employee’s PERSONAL expense. U. S. Taxpayer’s will not be subject to payment of legal bills for incompetent or dishonest personnel with regards to Governmental Employment.
The above steps should make for an excellent start to prevent veterans from being #RimadOut.
And We Do the Hokey Pokey and We Turn It All Around….
VA Dr.: Do the Hokey Pokey and turn it around for the Pokey, Pokey.
number 2 makes number 9 pointless. take the “IMMEDIATE LIFETIME DISMISSAL FROM ANY/ALL GOVERNMENTAL EMPLOYMENT” add “FEDERAL, STATE, OR MUNICIPAL”. Tack it on the end of number 2.
Not convinced. PPPPPPP. Sequence. Context. Last time I checked, Ex Post Facto was a BIG NO NO.
Ben?
┈┈┈┈┈┈┈┈┈┈┈What? You want
┈┈╱▔▔▔▔▔╲┈┈┈Us to do our
┈╱┈┈╱▔╲╲╲▏┈┈┈┈┈Jobs?
╱┈┈╱━╱▔▔▔▔▔╲━╮┈┈
▏┈▕┃▕╱▔╲╱▔╲▕╮┃┈┈
▏┈▕╰━▏▊▕▕▋▕▕━╯┈┈
╲┈┈╲╱▔╭╮▔▔┳╲╲┈┈┈
┈╲┈┈▏╭━━━━╯▕▕┈┈┈
┈┈╲┈╲▂▂▂▂▂▂╱╱┈┈┈
┈┈┈┈▏┊┈┈┈┈┊┈┈┈╲┈
┈┈┈┈▏┊┈┈┈┈┊▕╲┈┈╲
┈╱▔╲▏┊┈┈┈┈┊▕╱▔╲▕
┈▏┈┈┈╰┈┈┈┈╯┈┈┈▕▕
┈╲┈┈┈╲┈┈┈┈╱┈┈┈╱┈╲
┈┈╲┈┈▕▔▔▔▔▏┈┈╱╲╲╲▏
┈╱▔┈┈▕┈┈┈┈▏┈┈▔╲▔▔
┈╲▂▂▂╱┈┈┈┈╲▂▂▂╱┈
……..VAOIG/DOJ
You raise a good point about DBCs. After the VA has been shown repeatedly to be unable to follow their own policies, what makes anyone think they follow their policy on DBCs? I bet that process is even more grab-ass than reporting quack doctors.
Comments are closed.